Physiotherapy for Painful Radiculopathies
Peripheral neuropathic pain is common with an estimated population prevalence of 6.9%-10%. Currently, treatment of this condition largely depends on pharmacology, however with modest effects. This narrative review aimed to describe the current evidence for physical therapy in patients with chemotherapy-induced peripheral neuropathy (CIPN) and radicular pain.

Jesson et al (2020)
Peripheral neuropathic pain is common with an estimated population prevalence of 6.9%-10%. Currently, treatment of this condition largely depends on pharmacology, however with modest effects. This narrative review aimed to describe the current evidence for physical therapy in patients with chemotherapy-induced peripheral neuropathy (CIPN) and radicular pain.
Physiotherapy for Chemotherapy-Induced Peripheral Neuropathy
Key mechanisms in developing CIPN include microtubule disruption, mitotoxicity, and the neuroimmune response. They experience pain or a combination of numbness, tingling, or hot or cold sensations. This review described the aforementioned symptoms with the umbrella term “CIPN pain”.
Natural history is favorable in two-thirds of patients.
Prevention of CIPN
Several studies investigated the preventative effect of predominantly exercise. However, no meaningful effects to this date were found.
Treatment of CIPN
Some studies suggest an easing of symptoms due to exercise. Studies were small and had a modest to high risk of bias, meaning further research is required to confirm this hypothesis.
Effects of QOL
Effects look similar to those of the treatment of CIPN. Although even more research is required in this field.
Physiotherapy for Radicular Pain
The underlying mechanism of radicular pain is caused by mechanical or chemical irritation of spinal nerves or nerve roots, mostly cervical and lumbar. Natural history is favorable in two-thirds of patients. Common causes are disk herniations, spinal canal stenosis, and spondylolisthesis. One would think symptoms would occur in the corresponding dermatome, yet extra dermatomal pain is more often the rule, rather than the exception.
CENTRAL SENSITIZATION IN PATIENTS WITH PERSISTENT PAIN: FROM THE LAB TO THE CLINIC
Learn to Provide the Best Evidence-based Care to Help Patients with Chronic Pain

Stabilization and Motor Control
When compared to no or minimal care (such as TENS), spinal stabilization and/or motor control exercises provide some benefit. Although most trials report the aforementioned benefit, this clinically meaningful difference disappeared in the only trial with a low risk of bias (Hahne et al 2017).
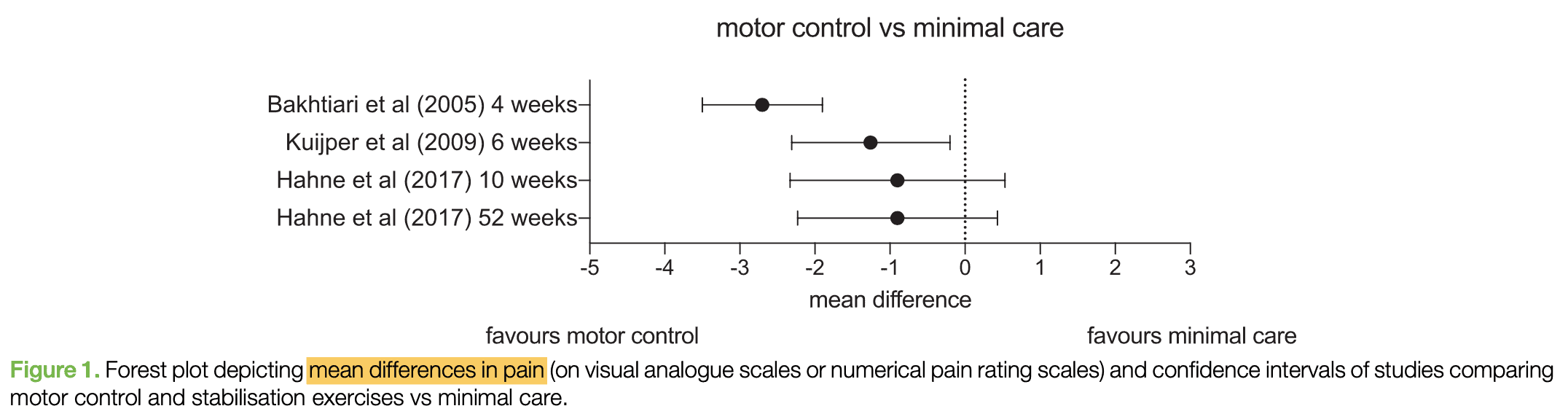
When stabilization and motor control exercises are compared to more substantial care (such as general exercises), there’s no evidence to suggest one is superior to the other.
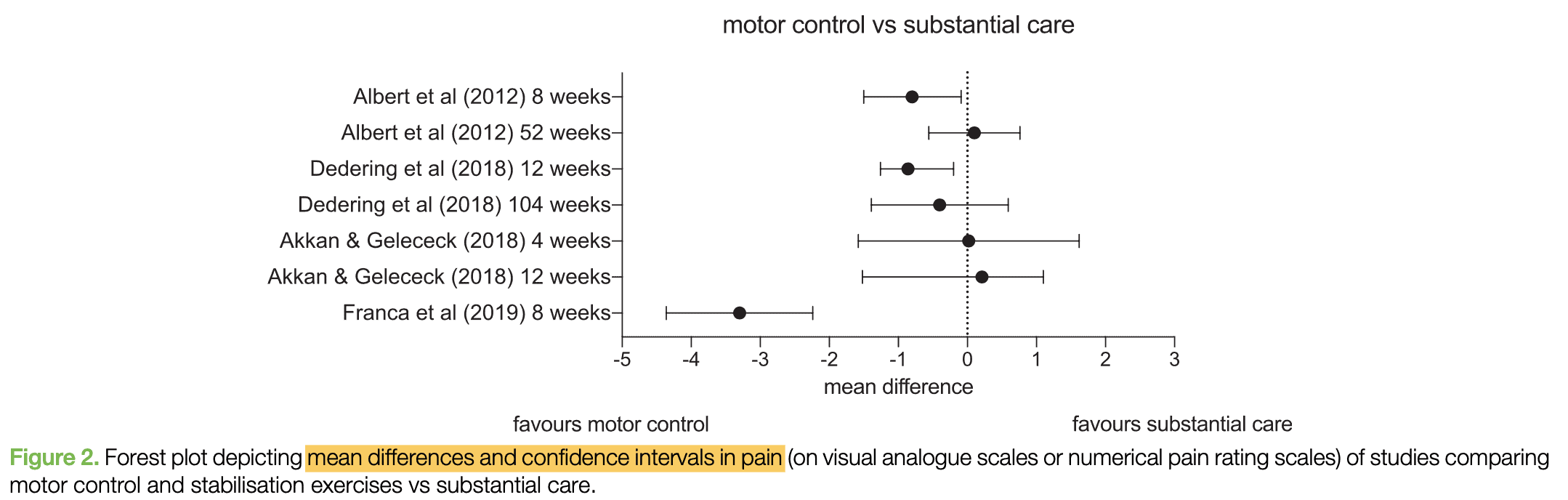
Interventions Directed at Neural Mechanosensitivity
“Physiotherapeutic techniques addressing neural mechanosensitivity include specific movements of peripheral nerves in relation to their surrounding tissues (neural sliders and tensioners) of interface techniques that are directed at the tissue surrounding the nerve.”
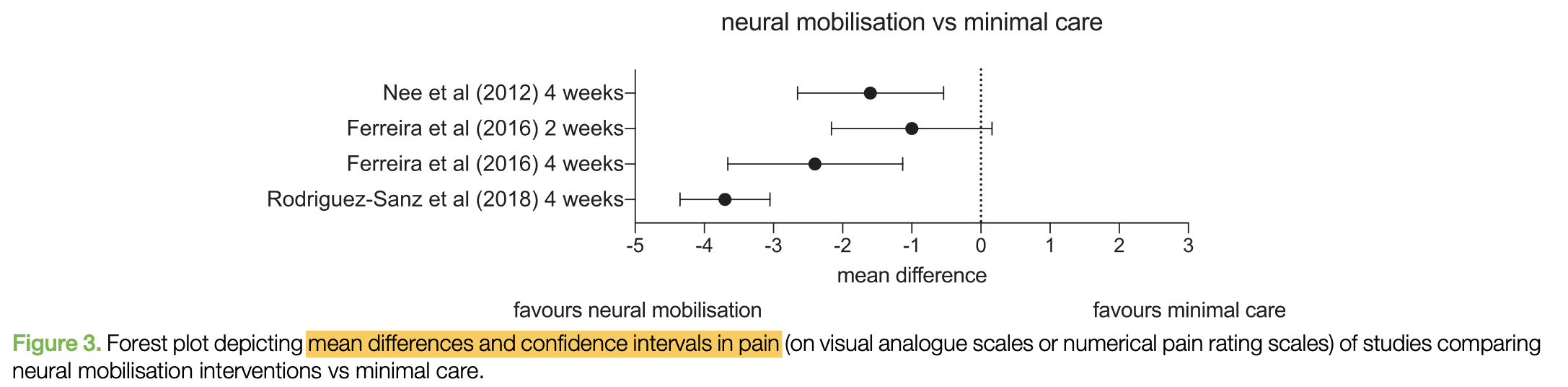
Similar to stabilization and motor control exercises, these techniques provided additional benefits compared to no or minimal care. When compared to substantial treatment, results were mixed with a large range of plausible outcomes. This conclusion is in conjunction with a recent systematic review (Su and Lim 2016).
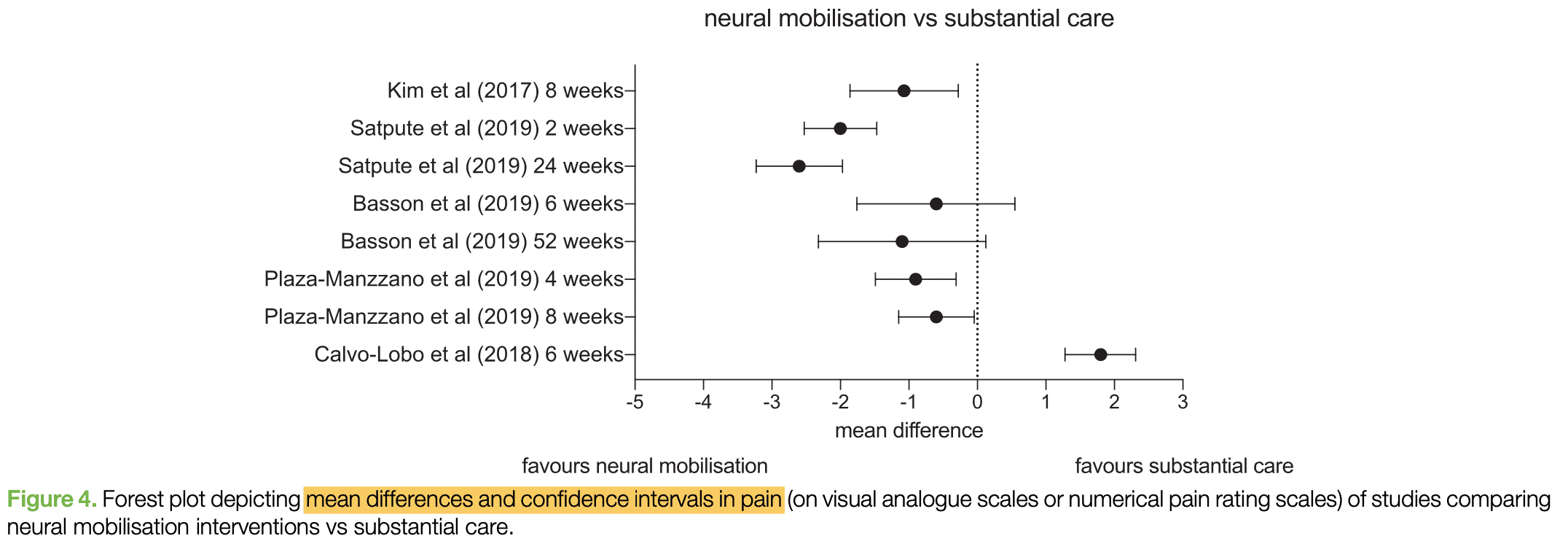
Effects of Physiotherapy on Disability for Radicular Pain
Trends for the effectiveness of physiotherapy on pain and disability were similar although disability decreased to a lesser extent. When disability is improved, pain improves as well. When pain improved, disability wasn’t necessarily better.
Do you want to know how to treat lumbar spinal stenosis conservatively? Be sure to watch this video!
References:
Jesson et al (2020): https://pubmed.ncbi.nlm.nih.gov/33490836/
Hahne et al (2017): https://pubmed.ncbi.nlm.nih.gov/27765714/
Su et al (2016): https://pubmed.ncbi.nlm.nih.gov/26710222/

Max van der Velden
Research Manager
NEW BLOG ARTICLES IN YOUR INBOX
Subscribe now and receive a notification once the latest blog article is published.







