Proximal Hamstring Tendinopathy | Diagnosis & Physio Treatment

Proximal Hamstring Tendinopathy | Diagnosis & Physio Treatment
Introduction & Epidemiology
Whereas proximal hamstring injuries are less frequent with sports engagement, musculotendinous junction injuries are more frequent. These injuries have a wide variety of appearances, from complete proximal avulsion injuries to partial-thickness tears to persistent insertional tendinopathy. These injuries frequently go undiagnosed or are treated slowly because of their low incidence and diverse appearance, which leads to extended periods of incapacity. In order to increase knowledge, speed up diagnosis, and ensure effective care, this blog post will explain the normal presentation, physical examination, diagnostic imaging, and therapeutic treatment choices for each of these entities (Degen 2019).
Proximal hamstring tendinopathy is most prevalent among fast walkers, distance runners, sprinters, and athletes performing change-of-direction activities such as football, soccer, or hockey.
Clinical Presentation & Examination
If you are a regular visitor to our webpage, then you might have seen or watched our video on 6 tips to diagnose lower limb tendinopathy.
Lower limb tendinopathy can be diagnosed with the help of the following 6 points:
- Epidemiological data (see above)
- Highly localized pain at the tendon enthesis
- Muscle wasting
- Hallmark signs
- Pain onset 24 hours after high+fast load activities
- A proportional load-pain relationship.
In this blog, we will specify those 6 points for the proximal hamstring tendon and look at possible differential diagnoses.
Palpation
Palpation should confirm well-localized pain at the ischial tuberosity. Be aware that proximal hamstring tendinopathy is one of the few tendinopathies that can present with diffuse referred pain to the back side of the hamstrings as well. As with other tendinopathies, symptoms usually become less prominent after a short warm-up period. The pain location requires an extensive differential diagnosis.
Differential Diagnosis
Differential diagnoses, with more diffuse symptoms are:
- Sacroiliac joint pain which can be in and excluded with the Cluster of Laslett.
- Referred pain from the lumbar facet joints of commonly L4/L5 and especially L5/S1, which can be examined by 3D extension PIVMs and PA provocation testing.
- The sciatic nerve can become irritated in the deep gluteal area, so what was formerly called piriformis syndrome and nowadays called deep gluteal syndrome.
- Next to palpation of the deep gluteal muscles, there are a couple of tests to help with this diagnosis of exclusion which all stretch or contract the deep gluteal muscles to entrap the sciatic nerve. You can also perform neurodynamic tests such as the Slump test which you’d expect to show up with positive findings
- Furthermore, in female runners with pain medial to the ischial tuberosity we have to take an Ischial ramus stress fracture into account. The diagnosis can ultimately only be made by imaging.
- In adolescent kicking athletes we have to take apophysitis into account and in post-adolescent athletes, in their 20s and 30s an unfused growth plate could be responsible for non-response to conservative therapy
- In the case of acute onset, we have to consider partial and full ruptures of the proximal hamstring tendon into account, which often happen with an audible pop in extreme hip flexion combined with knee extension.
- At last, a patient can suffer from Ischiofemoral impingement, which happens when the lesser trochanter of the femur impinges against the ischial bone during external rotation of the hip.
Muscle Wasting
In the case of proximal hamstring tendinopathy, the literature describing atrophic changes is sparse. As a general rule of thumb for tendinopathy, the muscle of the affected tendon and the muscles of the kinetic chain distal to that muscle are affected. To examine muscle wasting in this case, observe the hamstrings and calves for muscle bulk and differences and palpate them for tone, which is often reduced if patients have not been using them much.
Hallmark Sign
The hallmark sign of proximal hamstring tendinopathy is sitting pain on the tendon insertion as it is getting compressed between the sitting surface and the ischial tuberosity.
Pain onset/exacerbation 24 hours after high-load activities
Pain onset or exacerbation 24 hours after high+fast load activities: In the case of the proximal tendon you have to specifically ask for an increase in volume, intensity, or frequency of sprinting, lunging, hurdles, or hill running which has led to the onset of symptoms. This is often the case after a prolonged break as well. And secondly, the pain usually increased 24 hours after those high and fast load activities. Be aware that activities that require static stretching such as yoga or pilates and even simply sitting can induce tendinopathy as well.
Proportional Load-pain relationship
Like with every tendinopathy you are looking for an increase in pain with an increase in load on the proximal hamstring tendon. A good starting provocation test can be a double-leg bridge, followed by a single-leg bent knee bridge. Then continue with a bridge with a long lever and progress to higher load and speed like in catches for example. A very intense test is asking a patient to perform a double-leg deadlift, which is again progressed to a single-leg version with added load and speed. Pain levels have to increase with increasing difficulty, so if the single-leg bridge was scored with a 3 out of 10, a long lever bridge with added load and speed should be higher with the highest scores at single-leg deadlifts with added load and speed.
The literature describes 3 common orthopedic tests to diagnose proximal hamstring tendinopathy. They are:
WHAT TO LOOK FOR TO PREVENT HAMSTRING, CALF & QUADRICEPS INJURIES

Treatment
Unlike Achilles and patellar tendinopathy, proximal hamstring tendinopathy is less prevalent. For this reason, we are not aware of any randomized controlled trials evaluating the effectiveness of a progressive loading program like the ones we have presented for Achilles and patellar tendinopathy. Although high-level evidence is scarce, rehab principles are identical. The following rehab exercises are inspired by different expert opinions from Jill Cook and Peter Malliaras as well as a clinical commentary by Tom Goom and colleagues. A possible 4-stage rehab program can look like this:
Let’s have a closer look at each rehabilitation stage:
Management – Pain modification
Like with other lower limb tendinopathies load modification is critical in order to decrease pain and irritability. Especially energy storage loads should be limited to activities that can be carried out with tolerable pain and with increases in pain levels that settle within 24 hours. In a highly irritable tendon, it can be helpful to:
- Limit hamstring stretching if painful
- Modify sitting: A special hamstring cushion can help or sitting on a rolled-up towel so weight bearing is mainly on the posterior thighs instead of the ischium, sitting with a posterior pelvic tilt is preferable, or sitting on a higher chair
- Squatting in daily function should also be limited if painful
As with other lower limb tendinopathies, a progressive loading program is key to recovery. To monitor pain and determine load tolerance, you can use a load test like the short or long-lever bridge at the same time daily. The patient carries out the test and rates the pain level for 1 repetition.
As mentioned earlier, all exercises should be carried out with tolerable pain levels and an increase in pain should settle within 24 hours. If this is not the case, this means that the patient is not load-tolerant to those exercises yet.
Stage 1: Isometric
Goal: mainly to decrease pain or in case the patient is pain tolerant to isotonic loading, 2-3x per day, isometrics can be continued throughout the rehab program on off days if effect positive
Start in positions with the least compression of the proximal hamstring tendon against the tuber ischiadicum (0° hip flexion)
- Straight leg pull-down with elastic band
- Isometric trunk extension
- Isometric leg curl machine 45°, 45s x5 of at least 70% of MVC. Home variation: Isometric leg curl with a band (heaviest possible), point toes, posterior pelvic tilt
- Bridges (short & long levers): double, double with one leg shorter (load bearing, offset bridge), then single leg 🡪 long lever from low to high and completely straight knee

Stage 2: Isotonic Rehab (restricted hip flexion)
Isotonic rehab exercises can be performed in restricted hip flexion. The goal in this phase is to restore hamstring strength and muscle bulk and capacity in functional ROM. Start with limited hip flexion, 3-4 sets x 15 reps, progressed to 6-8 every other day with a 3-0-3 cadence. Use a metronome if patients struggle with speed.
Exercise examples:
- Prone hip extension (with or without theraloop)
- Hamstring Curls (better in prone lying): If a patient is not able to perform concentric exercises, you could opt to focus on eccentrics, the best way to isolate the hamstrings
- Bridging: When 15-20 reps are easy, progress, same progressions as isometric, start with the most challenging with acceptable load tolerance
- Eccentric bridge slides
- Nordic hamstrings, good for high-speed running

Stage 3: Isotonic Rehab into flexion
In this stage, it can be commenced when isotonic exercises in restricted hip flexion are tolerated. Dosage and loading parameters are identical to stage 2.
Example exercises are:
- Hip thrusts without/with weight, double and single leg
- Step-ups, which are a better option for sedentary and older people, increase the weight to 30kg 🡪 Progress with step height (Romanian)
- Deadlift (for athletes): straight knee, back straight, progress to about 30-35kg with DB, then use bar 🡪 progress to single-leg also called diver
- Alternative: Cable pull-down (straight knee, back straight)
- Split Squats (load up to BW) or lunges
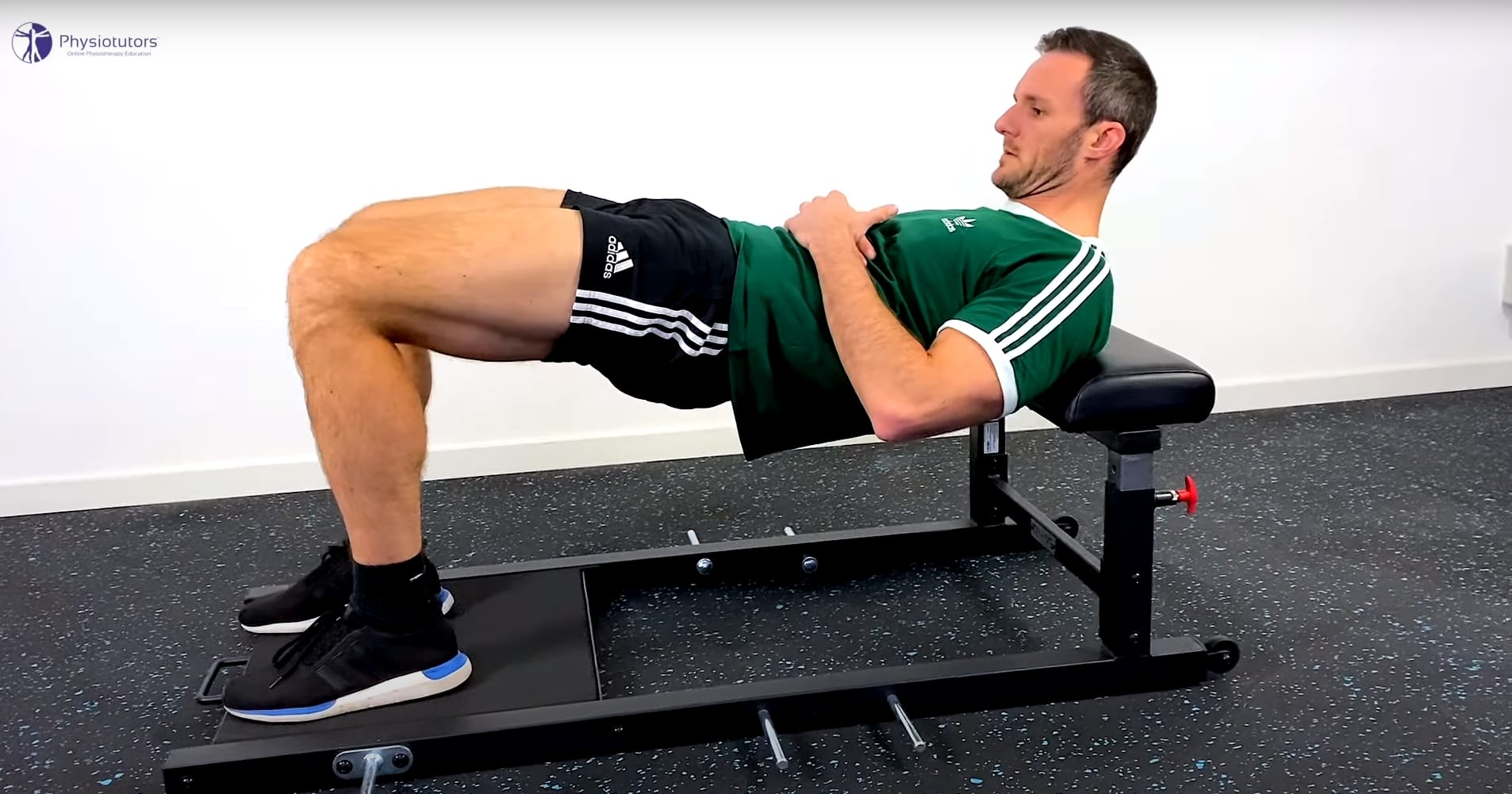
Stage 4: Energy storage exercises
This stage is only required for athletes returning to sports requiring energy storage and impact loading. Exercises can be performed every 3rd day. The requirements to start this phase are similar bilateral strength in single-leg exercises of stages 2 and 3 as well as the adequate execution and control of energy storage exercises.
Example exercises are:
- Variable hops: double leg, single leg, forward, backward, sideways, on a stepper, a skips
- Resisted running or Fast sled push or pull
- Kettlebell swings
- Alternate leg split jump

At last, graded return to sport can be started as soon as the patient is load tolerant to energy storage exercise progressions that replicate the demands of his or her sport in regard to volume and intensity of relevant energy-storage functions. Return to competition is allowed as soon as the patient is load tolerant to full training.
Do you want to learn more about how to treat tendons? Then check out our blog articles:
- 6 Risk factors for tendinopathy You Need to Know (#5 might surprise you!)
- Isometrics – A Wonder Weapon to Decrease Pain?
- 7 Crucial Facts You Didn’t Know about Tendons
References
THE BIG 3 - ADVANCED REHABILITATION OF HAMSTRING, QUADRICEPS, AND CALF MUSCLE- AND TENDON INJURIES


What customers have to say about this course
- Ivo Rigter11/07/25The Big 3 Prima informatieve cursus
 Rik06/06/25Perfect course Perfect course. Provides a comprehensive overview of diagnosis, prevention, and evidence-based rehabilitation of 'the big 3'. Thanks!
Rik06/06/25Perfect course Perfect course. Provides a comprehensive overview of diagnosis, prevention, and evidence-based rehabilitation of 'the big 3'. Thanks! - Anna Fabschitz30/03/25GREAT COURSE The course is very informative - a lot of knowledge, exercises, tipps, a great structure,...
I can highly recommend the course! 🙂 David Norenlind09/02/25Fantastic course on the topic of muscle and tendon injury The course does a great job of summarizing the research in the field and Enda provides clinical expertise along the way. A must-do course for anyone wanting to deepen their knowledge of muscle and tendon injuries.
David Norenlind09/02/25Fantastic course on the topic of muscle and tendon injury The course does a great job of summarizing the research in the field and Enda provides clinical expertise along the way. A must-do course for anyone wanting to deepen their knowledge of muscle and tendon injuries. - Senne Gabriëls25/12/24Worth the investment! This was my first online experience with courses. It was a very comprehensive and complete course. Management of tendon and muscle conditions in the lower limb became very clear in a way that no stone remained unturned.Eric van Bree09/12/24revalidatie onderste exstremiteiten zeer nuttig om je inzicht te vergroten bij revalidatie van sporters met klachten aan de onderste extremiteiten
- Ruben06/12/24Awesome info I really enjoyed the course. Could not recommend it enough!Thessa Budding06/12/24BIG 3 Interessant en meteen toepasbaar in de praktijk!
- Joris Bonarius25/11/24Informative and Efficient A very usefull course as an sportsphysio. Focussing on all important factors in injury risk, prevention, rehab and more!Pete23/11/24Course Summary I thought the course presented great content and was well organized. The format moving from general to injury specific was easy to follow. It could have been helpful to have a few more narrative sections, especially for the Case studies. Being in a High Performance setting, the course also allowed me to get some confirmation bias while at the same time providing the foundational understanding of tissue biology. The exercises and progressions also provided an alternative for the clinician and performance specialist.
 Bas Slieker, Physiotherapist02/10/24Well-structured, evidence-based and clinically relevant. The course strikes a perfect balance between clear explanations, evidence and practical tools. It highlights the complexity of tendon and muscle rehab and provides a structured way to integrate biopsychosocial factors. Highly recommended.Pascal Van de Kamp24/09/24Very structured, thanks Very structured, covering everything from anatomy to injury to rehab and movement patterns. Quizes were a bit annoying after every chapter. Still enjoyed it, refreshing course to stay sharp in my rehab plans.
Bas Slieker, Physiotherapist02/10/24Well-structured, evidence-based and clinically relevant. The course strikes a perfect balance between clear explanations, evidence and practical tools. It highlights the complexity of tendon and muscle rehab and provides a structured way to integrate biopsychosocial factors. Highly recommended.Pascal Van de Kamp24/09/24Very structured, thanks Very structured, covering everything from anatomy to injury to rehab and movement patterns. Quizes were a bit annoying after every chapter. Still enjoyed it, refreshing course to stay sharp in my rehab plans. Gustav Hübinette30/01/24The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries REVIEW OF THE BIG 3
Gustav Hübinette30/01/24The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries REVIEW OF THE BIG 3
I experienced the course as very well-structured, maintaining a clear thread throughout the entire program. The content is clearly based on updated evidence, providing numerous valuable tips and tricks for implementing rehabilitation of THE BIG 3.
What I had wished for to be different is to include more recorded lectures, as there is currently a considerable amount of test-based information. Yoran Deleu30/12/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries Well structured course from the theoretical background to clear practical exercises needed for rehabilitation!
Yoran Deleu30/12/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries Well structured course from the theoretical background to clear practical exercises needed for rehabilitation! Adam Stewart14/11/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries VERY THOROUGH AND EXCELLENT JOB USING EVIDENCE BASED PRACTICE
Adam Stewart14/11/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries VERY THOROUGH AND EXCELLENT JOB USING EVIDENCE BASED PRACTICE
Enda does a great job with this course and dives into as much detail as you would like throughout. Excellent job of keeping the most up-to-date information in the presentation. Takes time to get through it all, but very worth it Olivier Gouvernet11/10/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries BIG §
Olivier Gouvernet11/10/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries BIG §
The course is very well structured, the anatomical reminders are relevant, each stage of rehabilitation is well detailed and the videos of the exercises make it easy to see and understand what needs to be monitored and done.
In my opinion, the last phases of rehabilitation are the most interesting, as they are rarely covered. This helps to reduce the gap between the load at the end of treatment and the load of a return to sport. Jeremy Beyer05/09/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries An excellent course on the rehabilitation and management of lower extremity muscle & tendon injuries! Enda covers serious range in this course with lessons on muscle & tendon physiology all the way to late stage rehab and discussions around power & reactive strength development. This course is comprehensive and covers many of the overlooked aspects of muscle and tendon rehab. Enda highlights foundational rehabilitation concepts in an easy to digest manner that is guaranteed to influence the way you practice.
Jeremy Beyer05/09/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries An excellent course on the rehabilitation and management of lower extremity muscle & tendon injuries! Enda covers serious range in this course with lessons on muscle & tendon physiology all the way to late stage rehab and discussions around power & reactive strength development. This course is comprehensive and covers many of the overlooked aspects of muscle and tendon rehab. Enda highlights foundational rehabilitation concepts in an easy to digest manner that is guaranteed to influence the way you practice. Beppeke Molenaar04/05/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries EXCELLENT COURSE, INCREDIBLY KNOWLEDGEABLE
Beppeke Molenaar04/05/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries EXCELLENT COURSE, INCREDIBLY KNOWLEDGEABLE
This is a fantastic course, with loads of information that is very applicable to daily practice.
I think this course has offered me the most in terms of learning and professional development out of all the courses I’ve done so far.
The set-up of the course is really well-structured. The videos are clear, the information in the text is evidence-based, very in-depth, and at the end of each unit, you can find further readings for anyone who wants to dive even deeper into the material.
I would highly recommend this course! Badrinath31/03/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries The presentation is quite evidence based and evidence informed. It is presented in a structured manner. The author has put lots of effort. It is an application based course.
Badrinath31/03/23The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries The presentation is quite evidence based and evidence informed. It is presented in a structured manner. The author has put lots of effort. It is an application based course. Frederik Adriaensens30/12/22The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries VERY NICE OVERVIEW OF ALL THE INFLUENCIAL MECHANICS AND REHAB OPTIONS
Frederik Adriaensens30/12/22The Big 3 - Advanced Rehabilitation of Hamstring, Quadriceps, and Calf Muscle- and Tendon Injuries VERY NICE OVERVIEW OF ALL THE INFLUENCIAL MECHANICS AND REHAB OPTIONS
Thanks for the excellent refresher!