Pain Trajectories Following High versus Low Loading of Hypermobile Shoulders

Introduction
People with hypermobile spectrum disorders who experience shoulder pain are often referred to physiotherapy, but no superior treatment has yet been found. In 2022, we covered a randomized controlled trial by the same author, where the short-term effectiveness of high-load strengthening in patients with hypermobile shoulders was studied. This RCT found statistical superiority for the high-load strengthening compared to low-load strengthening, but the improvements remained below the threshold for clinically relevant improvements. For certain participants, the high loading achieved important improvements in shoulder function, although patients and clinicians often fear high-load strengthening leading to pain flare-ups. Therefore, this secondary analysis delved into the pain trajectories to capture weekly pain fluctuations following high versus low loading of hypermobile shoulders.
Methods
This was a secondary analysis of data from a previously conducted randomized controlled trial (RCT). This trial was registered on ClinicalTrials.gov (NCT03869307). This trial compared a low-load versus a high-load strengthening program, focusing on self-reported functioning in patients aged 18-65 years with hypermobility spectrum disorder (HSD). Eligibility criteria for HSD included:
- Generalized HSD (G-HSD): Beighton score ≥ 5/9 for females ≤ 50 years, and ≥ 4/9 for females > 50 years and all males.
- Historical HSD (H-HSD): Beighton score 1 point below the age/sex-specific cutoff and positive self-assessment five-part questionnaire on hypermobility (5PQ) (≥ 2/5 positive answers).
Participants also required at least one of the following symptoms:
- Musculoskeletal pain in one or both shoulders for ≥ 3 months.
- Recurrent atraumatic joint dislocations or instability, defined as: (a) ≥ 3 dislocations in the same shoulder, (b) ≥ 2 dislocations in two different joints (≥ 1 in shoulder) at different times, and/or (c) medical confirmation of instability in ≥ 2 joints (≥ 1 in shoulder).
Participants were excluded if they had referred pain from the cervical spine, rheumatic, connective tissue, or neurological diseases, were pregnant or had given birth within a year or planned to get pregnant, had shoulder surgery within the past year, or a steroid injection in the affected shoulder in the past 3 months.
The participants were randomly assigned in a 1:1 ratio to either the HEAVY or LIGHT group. For both groups, the same pain threshold was established. The participants were informed that pain ranging from 0-2 was considered safe, 3-5 was acceptable, and pain above 5 was considered high risk. The exercises and loads were continuously adjusted to fit each participant individually. A pain level of 5 at baseline was safe, but no increase was tolerated. In case of symptoms exceeding the predefined levels, the sets and number of repetitions could be lowered, the loads or range of motion could be adjusted, or certain provoking exercises could be skipped, or the number of exercise sessions could be temporarily reduced.
All participants received education in scapular correction and joint protection adapted from the Danish Rheumatism Association.
The HEAVY group performed 5 exercises, twice weekly supervised and once weekly at home, using individually adjusted dumbbell loads up to 15 kg. Loading progressed from 50% of 10RM (3 sets of 10 repetitions) at week 1, progressing to 70-90% of 10RM in weeks 2-3, to 10RM in weeks 4-9, and 8RM (4 sets of 8 repetitions) in weeks 10-15, concluding with 70% 8RM in week 16 to allow for recovery before the final testing. The loads were continuously adjusted to fit the capabilities of the patient.
The exercises included side-lying external rotation (neutral), prone horizontal abduction, prone external rotation (90° shoulder abduction), supine scapular protraction, and seated scaption. Further program details are provided in the image below.
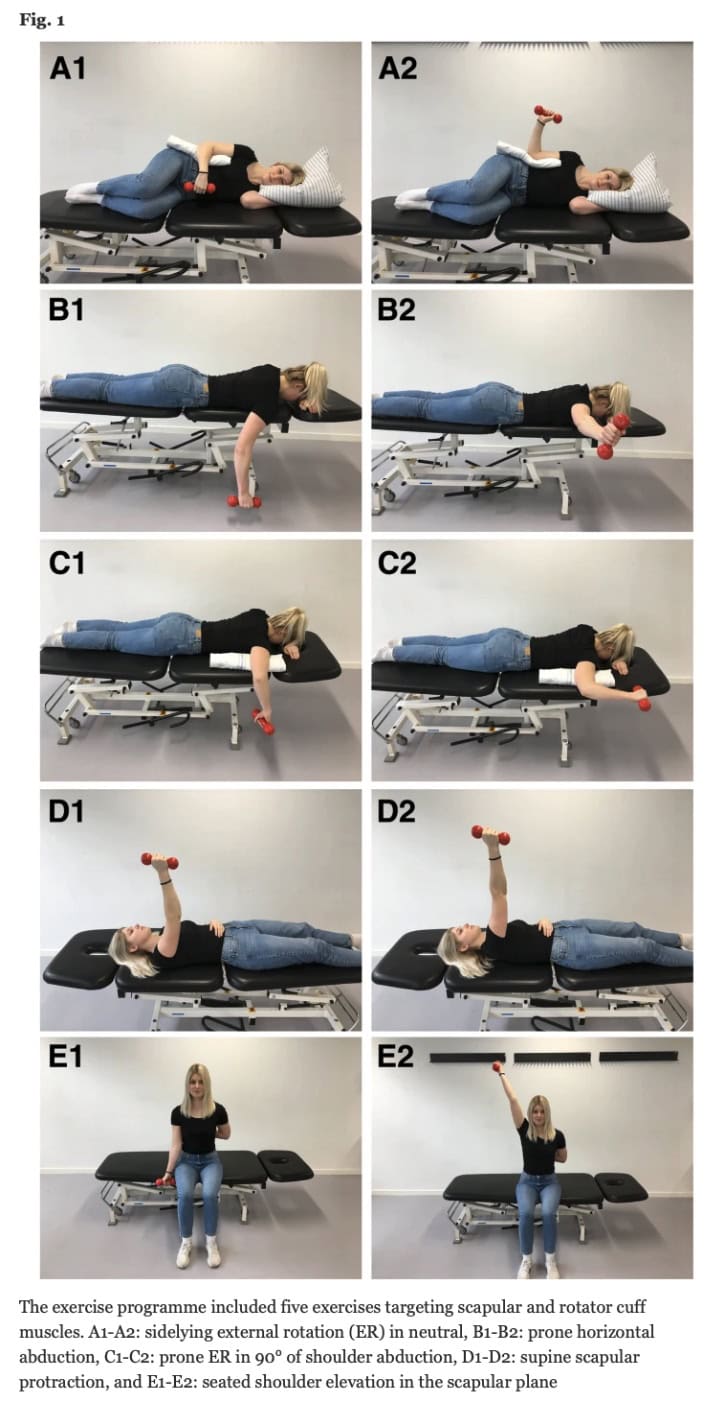
The LIGHT group mirrored standard Danish physiotherapy care, emphasizing three weekly self-training sessions during 16 weeks. Exercises were introduced initially, with supervised sessions at weeks 5 and 11 for new exercises. The program featured nine shoulder exercises across different phases:
-
- Phase 1 (week 1-4): Posture correction with scapula settings for 1 set of 10 repetitions.
- Phase 2 (week 5-10): Isometric shoulder abduction, internal/external rotation (90° elbow flexion) against a wall, and standing shoulder weight-bearing against a table. Two sets of 10 repetitions were performed per exercise.
- Phase 3 (week 11-13): using a yellow Theraband, shoulder abduction, internal/external rotation (90° elbow flexion), and four-point kneeling with single-arm raising were performed for 1 set of 10 repetitions.
- Phase 4 (week 14-16): The program of phase 3 was continued but for 2 sets of 10 repetitions.
Outcome Measures
Baseline demographics were collected, and shoulder function was assessed using the Western Ontario Shoulder Instability Index. Exercise logbooks were filled with the pain intensity before and after each exercise session. Pain trajectories were assessed using pre-exercise pain scores at the final session each week, reported via an 11-point Numerical Rating Scale (NRS) (0 = no pain, 10 = worst pain imaginable). Exercise-induced pain was evaluated as the change in pain before and after exercise, using the mean of the three sessions each week.
Results
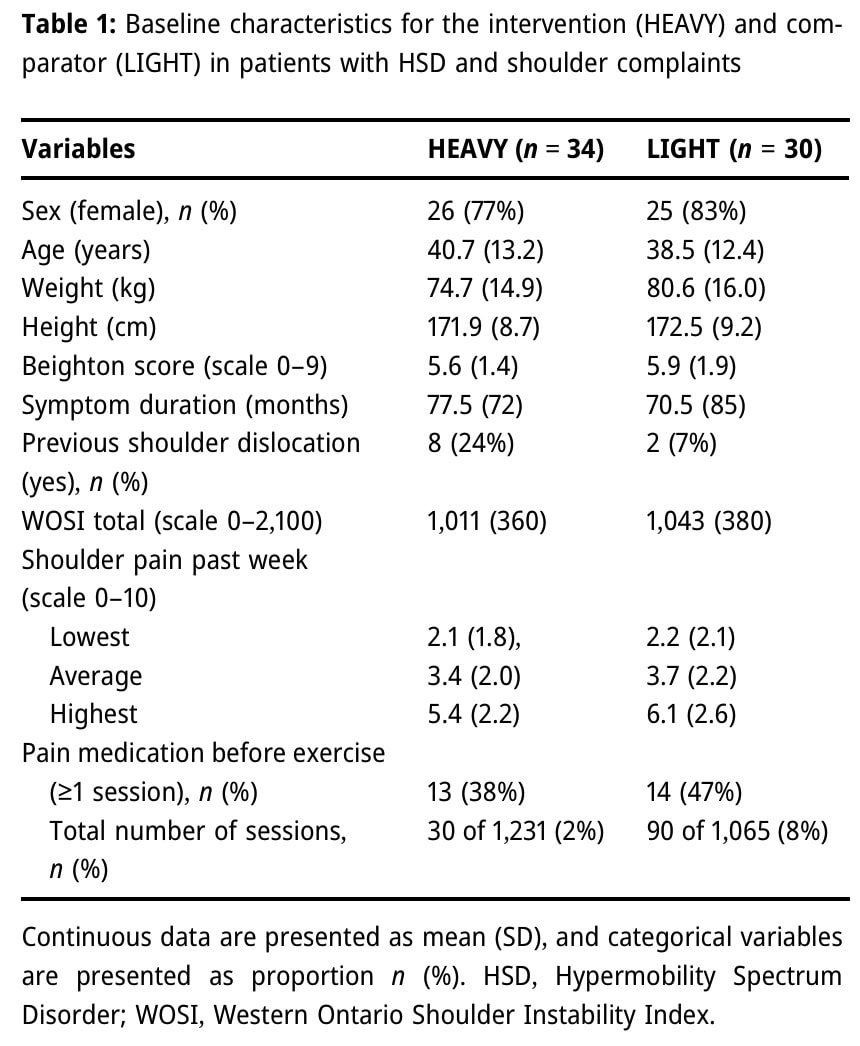
A total of 100 participants were included in the original study. Logbooks from 36 participants were lost to follow-up. Therefore, sixty-four participants provided data for this secondary analysis. Of them, 34 were randomized to the HEAVY group and 30 to the LIGHT group. Almost four out of five participants were female. Their mean age was 39 years, and their mean Beighton score was 5.8.
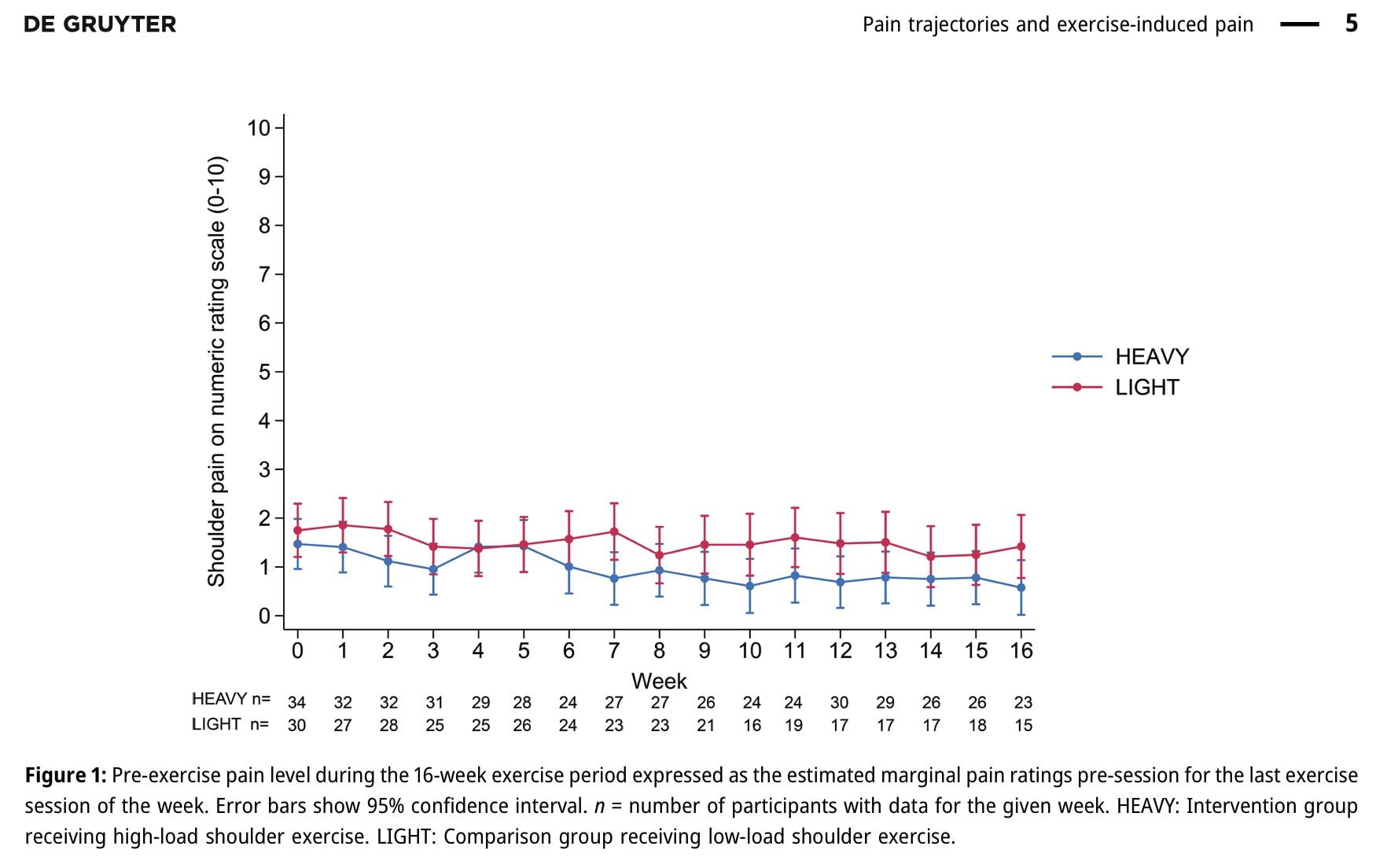
The analysis of the pain trajectories showed that pain in both groups reduced over the 16 weeks. The HEAVY group saw reductions of 0.89 on the 0-10 NRS scale, from 1.47 at baseline to 0.58 at 16 weeks. The LIGHT group achieved pain reductions of 0.33 NRS, from 1.75 at baseline to 1.42 at 16 weeks. This resulted in a between-group difference of 0.56 NRS, which was not statistically significant.
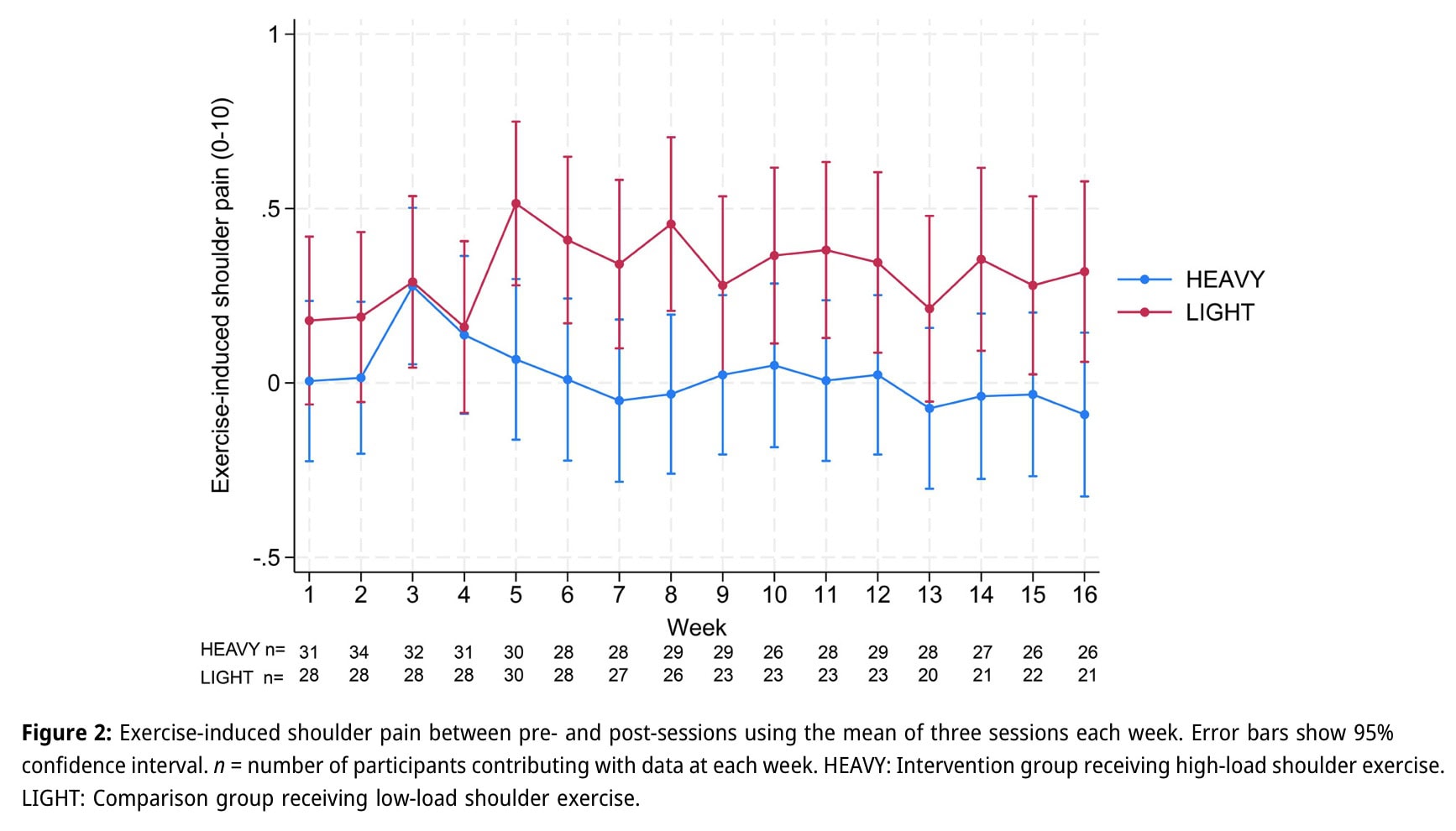
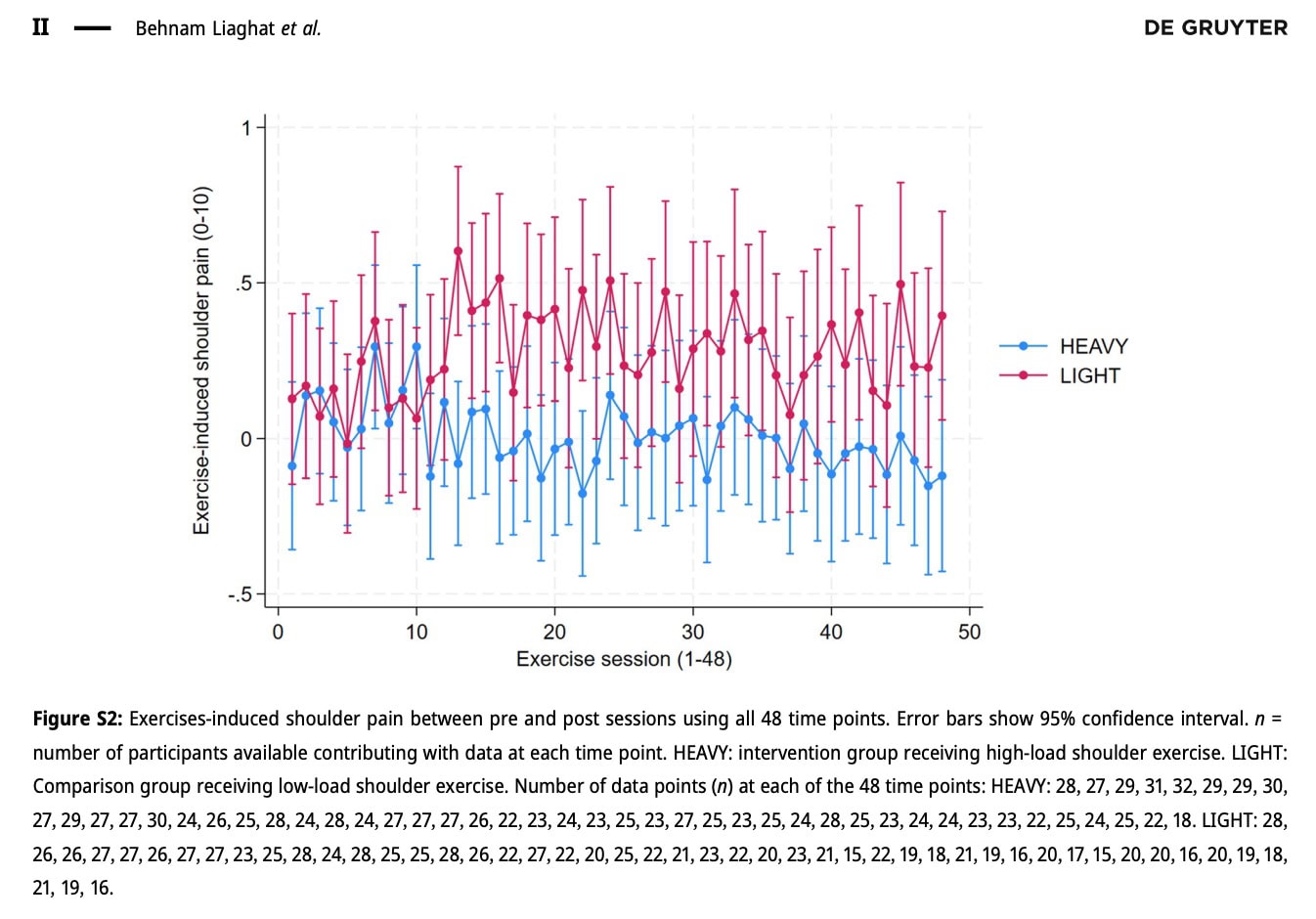
The analysis of the exercise-induced pain revealed similar pain over time in both groups. Both groups demonstrated low levels of exercise-induced pain, with averages below 0.5 NRS throughout the 16 weeks.
Questions and thoughts
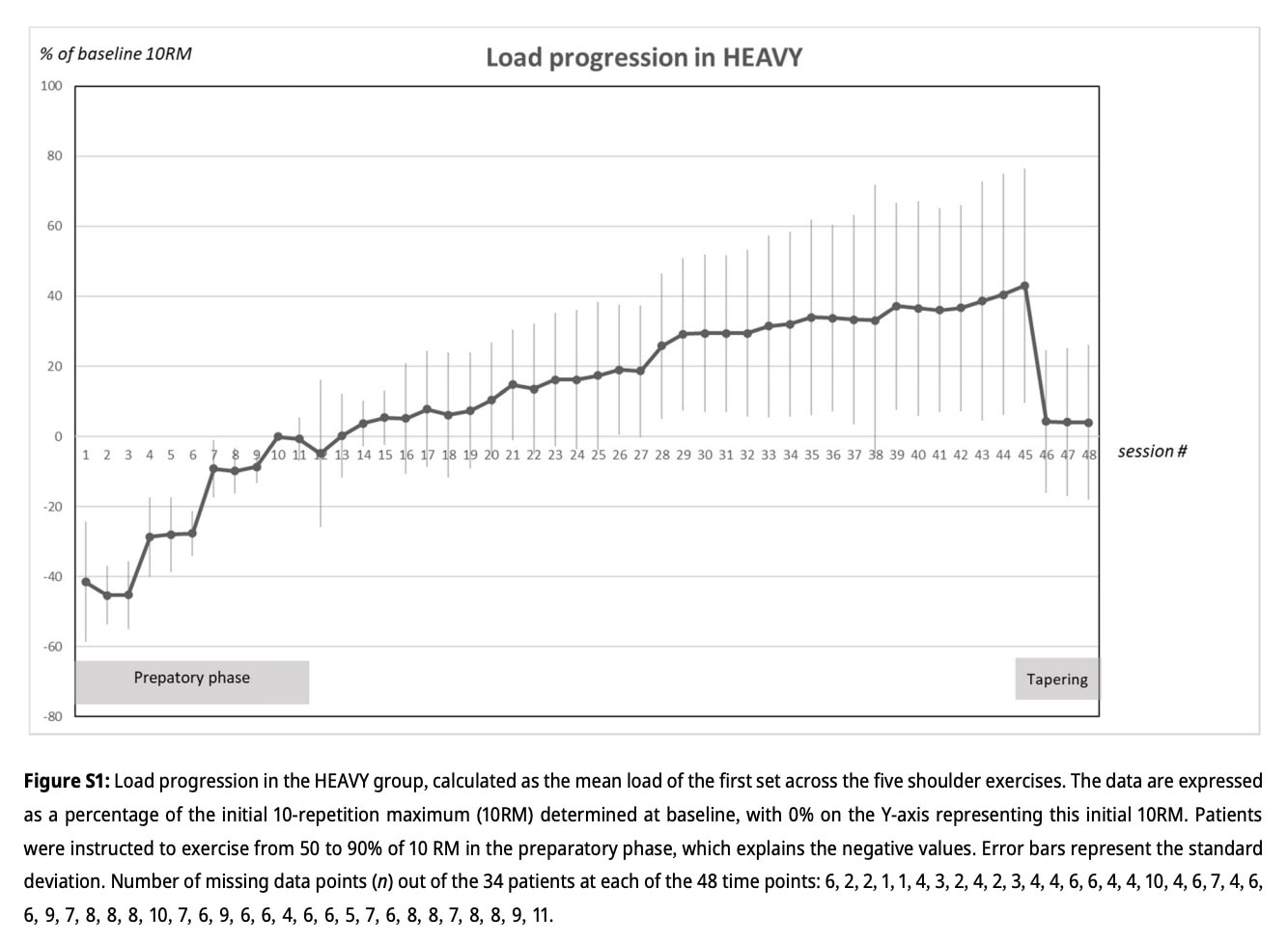
While no differences were observed between both groups in terms of pain fluctuations and pain scores improved likewise in both groups, loading of hypermobile shoulders in the HEAVY group showed a nice increase in weight tolerance over the weeks. The participants in the HEAVY group reached a peak mean of 43% above their baseline 10RM. Patients with HSD who need to improve their strength might achieve more benefit from the progressive increase in weight tolerance over the weeks. But no such graph or details were provided for those in the LIGHT loading of hypermobile shoulders group, so we have to remain cautious about this finding.
The LIGHT group’s standard care involved primarily unsupervised low-load exercises with limited in-person supervision. This resulted in a significant difference in how the groups were treated, apart from the intervention. This is a key problem for the validity of the results, as specified by the RCT checklist by Cochrane. You can wonder how much supervision is truly necessary for low-load programs in this population to ensure adherence and correct technique. Could more supervision and patient-therapist interaction have improved the LIGHT group’s outcomes?
As the study was about pain, other outcome parameters like shoulder, mobility, stability or fear of movement were not explored, despite being relevant for this population. The original trial found no differences in the function of the shoulder between low and high loading of hypermobile shoulders.
Talk nerdy to me
Two sensitivity analyses were performed: one where the intake of pain medications before exercise sessions was taken into account, and one where every session’s pain data were used instead of weekly mean values. Both analyses yielded similar results to the primary analysis’s findings.
An important limitation of the current study is the data loss of more than one-third of the total patient sample. As this is a secondary analysis, power is already lower since it was calculated to specifically answer the primary RCT’s question. A significant data loss on top of that may be endangering the conclusions made here.
Another limitation to bear in mind is the relatively low pain scores in this population at baseline. While this may seem encouraging at first, lower pain scores present a challenge for demonstrating significant pain improvement. As the mean pre-intervention scores were 1.47 and 1.75 out of 10 NRS, for the HEAVY and LIGHT groups, respectively, there was only a limited potential for the intervention to reduce pain. One possible explanation for the low pain scores observed may lie in the fact that the eligibility criteria specifically stated that participants were eligible for inclusion if they had either pain and/or mechanical shoulder symptoms. It is therefore plausible that some patients did not experience pain when they entered the study, but were more affected by mechanical symptoms. Likewise, no minimum pain threshold for inclusion was established. This altogether has impacted the clinical relevance of the study, as the aim was to observe pain fluctuations in this cohort.
Therefore, the generalizability of the findings is specifically lowered, and people with HSD and high pain scores may be left out in the dark. In individuals with HSD and low baseline pain scores, the study did not reveal differences between heavy and light loading of hypermobile shoulders, suggesting that patient preferences may be a key factor in treating this condition. Further investigations should take place to explore how those with more severe baseline symptoms would respond to heavy loading.
Take-home messages
This secondary analysis of a randomized controlled trial on low versus high loading of hypermobile shoulders did not result in differences in pain fluctuations between the two treatment options. Equal improvements in pain scores over the 16 weeks were observed between the groups. Exercise-induced pain remained below 0.5 out of 10 on the NRS scale in this study, but pain scores at baseline were already on the very low end of the spectrum, providing little room for improvement. Contrary to common beliefs or fears, high-load strengthening, when carefully monitored, did not result in larger exercise-induced pain compared with low loading of hypermobile shoulders.
A potential threatening limitation to the conclusions is the amount of missing data, particularly for exercise-induced pain, due to lost logbooks. While the statistical methods used can handle some missing data, a significant amount of missing information could reduce the study’s power to detect true differences between the groups, potentially leading to a false conclusion that the interventions are similar in their effect on exercise-induced pain when a difference might actually exist.
Reference
LEARN TO DISTINGUISH SHOULDER FACTS FROM FICTION
Awarded World Leading Shoulder Expert Filip Struyf takes you on a 5-Day Video Course to Bust Lots of Shoulder Myths that Prevent you From Delivering the Best Care for your patients with Shoulder Pain

