Medial Epicondylalgia / Golfer's Elbow | Diagnosis & Treatment
Medial Epicondylalgia / Golfer’s Elbow | Diagnosis & Treatment
Introduction & Epidemiology
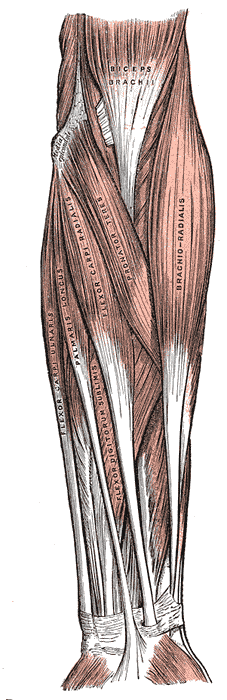 Medial Epicondylalgia, better known as Golfer’s elbow is a tendinopathy of the common wrist flexor and pronator muscle origin at the medial epicondyle. In comparison to its “big brother” tennis elbow, Golfer’s elbow is 4 to 7 times less common. A study by Leach et al. (1987) even mentions that LE is 7-10 times more common than medial epicondylalgia. In a study of the US military, the incidence rate for golfer’s elbow was 0.81 per 1000 person-years (Wolf et al. 2010).
Medial Epicondylalgia, better known as Golfer’s elbow is a tendinopathy of the common wrist flexor and pronator muscle origin at the medial epicondyle. In comparison to its “big brother” tennis elbow, Golfer’s elbow is 4 to 7 times less common. A study by Leach et al. (1987) even mentions that LE is 7-10 times more common than medial epicondylalgia. In a study of the US military, the incidence rate for golfer’s elbow was 0.81 per 1000 person-years (Wolf et al. 2010).
Medial epicondylalgia is thought to result from overuse of the common flexor-pronator tendon complex (including the pronator teres, flexor carpi radialis, palmaris longus, flexor digitorum superficialis, and the flexor carpi ulnaris). Excessive valgus stress has been implicated in the development of medial elbow pain as well (Mishra et al. 2014).
The term epicondylitis was questioned over time as histological studies have failed to show inflammatory cells (macrophages, lymphocytes, and neutrophils) in the affected tissue. These studies showed fibroblastic tissue and vascular invasion that lead to the term ‘tendinosis’. This rather defines a degenerative process characterized by an abundance of fibroblasts, vascular hyperplasia, and unstructured collagen (De Smedt et al. 2007)
Follow a course
- Learn from wherever, whenever, and at your own pace
- Interactive online courses from an award-winning team
- CEU/CPD accreditation in the Netherlands, Belgium, US & UK
Clinical Presentation & Examination
Elbow pain is the presenting complaint in patients with epicondylalgia. Patients often tend to ignore early symptoms and visit a health professional rather late. History describes either trauma or repetitive unilateral tasks at work, during ADLs, or sports with a gradual onset of pain (Orchard et al. 2011). The pain is usually worse with activity and relieved by rest and may or may not radiate down the forearm along the wrist flexor muscles. On top of that, patients might experience weakness in the hand and difficulty carrying items (Pitzer et al. 2014).
Although medial and lateral epicondylitis are similar, a study by Pienimäki et al. (2002) compared the two conditions in two chronic groups and found that the reduction in grip strength is less severe in medial epicondylalgia nd that pain is more widespread in lateral epicondylalgia.
Examination
For a thorough assessment and differential diagnosis, the cervical spine, shoulder, elbow, and wrist should be examined in both conditions. Patients with medial epicondylalgia present with tenderness at the origin of the common flexor-pronator tendon of the forearm, at or just distal to the medial epicondyle.
In the literature, only two orthopedic tests are described to assess medial epicondylalgia. Watch the videos below to learn how to perform them:
The second test, Polk’s Test, described by Polkinghorn et al. (2002) stresses both the lateral epicondyle in phase I of the test, as well as the medial epicondyle in the second phase of the test:
WATCH TWO 100% FREE WEBINARS ON SHOULDER PAIN AND ULNA-SIDE WRIST PAIN

Follow a course
- Learn from wherever, whenever, and at your own pace
- Interactive online courses from an award-winning team
- CEU/CPD accreditation in the Netherlands, Belgium, US & UK
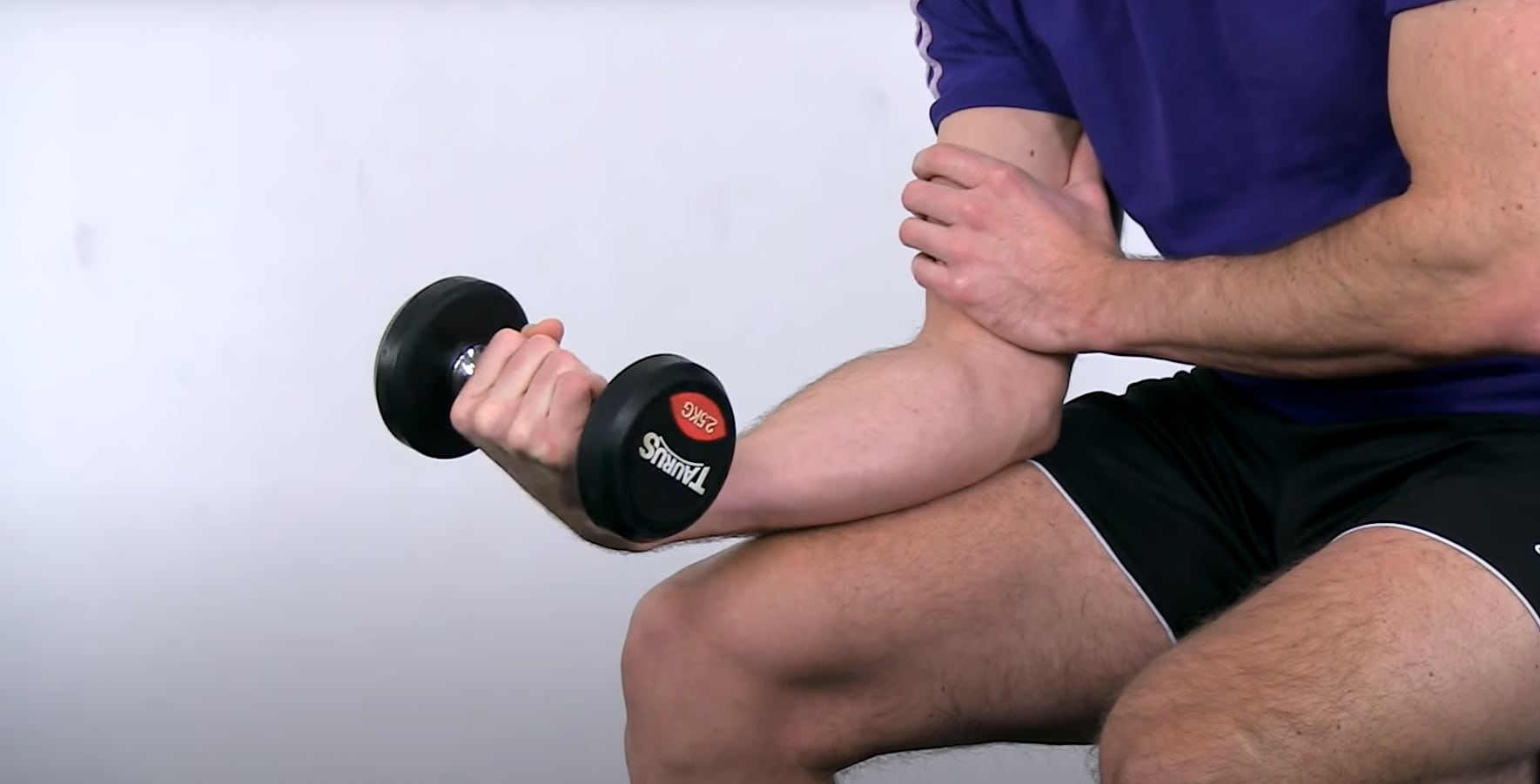 Like in other tendinopathies, the absolute basics for tendon rehab are slow and heavy resistance exercises. The go-to option to target the common origin of the wrist flexors are dumbbell curls with a weight that can be moved by the patient with tolerable pain for somewhere between 5-15 repetitions. If your patient doesn’t have dumbbells at home, he or she can use a backpack filled with weight or a water bottle. It’s important to stick to a cadence of no faster than 2-3 seconds up and 2-3 seconds down as we want a slow load applied to the tendon. Have the patient perform plus or minus 3 sets every other day. This frequency is derived from Magnussen et al. in the year 2010 who have shown that intense loading of tendons resulted in a net collagen degradation of up to 36 hours. However, the loads included in this study were huge like running for 36 kilometers. In my personal case, I prefer performing dumbbell curls on a daily basis for 3 sets with a weight that I can move around 10 times with tolerable pain. Try to challenge yourself or your patient and increase the number of reps and eventually the weight in the course of days and weeks.
Like in other tendinopathies, the absolute basics for tendon rehab are slow and heavy resistance exercises. The go-to option to target the common origin of the wrist flexors are dumbbell curls with a weight that can be moved by the patient with tolerable pain for somewhere between 5-15 repetitions. If your patient doesn’t have dumbbells at home, he or she can use a backpack filled with weight or a water bottle. It’s important to stick to a cadence of no faster than 2-3 seconds up and 2-3 seconds down as we want a slow load applied to the tendon. Have the patient perform plus or minus 3 sets every other day. This frequency is derived from Magnussen et al. in the year 2010 who have shown that intense loading of tendons resulted in a net collagen degradation of up to 36 hours. However, the loads included in this study were huge like running for 36 kilometers. In my personal case, I prefer performing dumbbell curls on a daily basis for 3 sets with a weight that I can move around 10 times with tolerable pain. Try to challenge yourself or your patient and increase the number of reps and eventually the weight in the course of days and weeks.



