Psychological exposure and outcomes in shoulder hypermobility

Introduction
A while ago, we reviewed the RCT by Behnam Liaghat et al. from 2022 which compared high-load versus low-load strengthening exercises in hypermobile shoulders. In this trial, the group performing high-load exercises improved more than the other group, but this difference did not attain the minimally clinically important difference in the primary outcome when analyzing it by intention-to-treat. The authors found, however, that the participants who followed the protocol did achieve the minimal important difference of 250 points on the WOSI questionnaire. Shoulder hypermobility is associated with more frequent reports of shoulder disability, pain, and reduced quality of life. This makes it possible that other factors than adherence are playing a role in treatment efficacy. Recent evidence indicates that psychological factors were consistently associated with outcomes from exercise-based treatment, yet the rationale up to now remains more focused on biological explanations. In this follow-up paper, the aim was to assess the association between several psychological exposure and outcomes in shoulder hypermobility. Therefore, the authors conducted a secondary analysis to reveal what psychological baseline characteristics were associated with a better outcome after 16 weeks of performing the exercises.
Methods
In this trial, a low-load strengthening program was compared against a high-load strengthening program for self-reported functioning in patients with hypermobility spectrum disorder (HSD). Let’s take a look at our research review of the study by Liaghat to get to know more about the study participants.
In brief, the high-load group received 5 exercises to perform 2x/w under supervision and 1x/w at home. The exercises were performed using dumbbells up to 15 kg, with individually adjusted loads. The exercises in the first 3 weeks were performed at an increasing load from 50% to 70%, to 90% of 10RM. Thereafter, from weeks 4-9 loads were increased to 10RM, and in weeks 10-15 sets were performed using loads of 8RM.
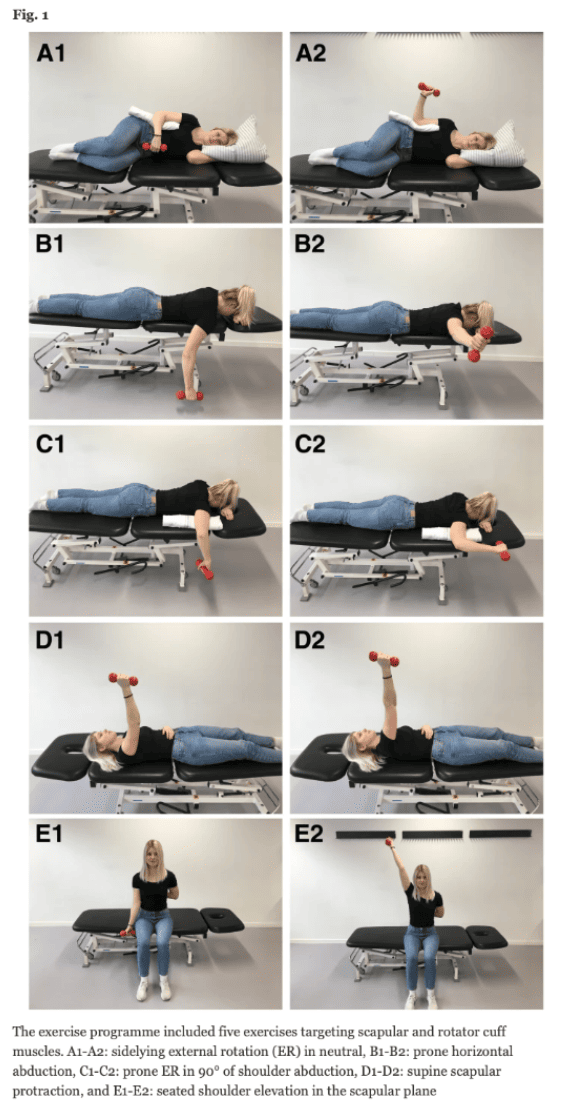
The low-load strengthening group performed self-training. In the study, exercises were introduced to the patients and they were supervised at weeks 5 and 11 when new exercises were done. Their program included nine shoulder exercises: posture correction, shoulder abduction, shoulder internal and external rotation with 90° flexion at the elbow joint against a wall, and standing weight-bearing in the shoulders against a table, shoulder abduction, shoulder internal and external rotation at 90° flexion at the elbow joint and four-point kneeling with single-arm raising.
For the inclusion criteria, I suggest you look at our previous review. At baseline, the following measurements were obtained:
- Patient expectations of treatment effect: measured by asking to rate on a 7-point Likert scale “How much do you expect your shoulder problem to change as a result of physiotherapy treatment?”. A score of zero represents that they expect their shoulder would be “worse than ever” and a score of six indicates they expect a complete recovery.
- Self-efficacy related to symptoms was assessed by the Self-Efficacy Questionnaire. This score ranges from 0-60 with higher scores indicating higher self-efficacy.
- Fear of movement was assessed using the Tampa Scale of Kinesiophobia 11. This score ranges from 11 to 44 with higher scores indicating higher fear of movement.
- Symptom duration
The association of these exposure variables was assessed on the outcome variables shoulder function (measured with Western Ontario Shoulder Instability Index – WOSI), pain (Numeric Pain Rating Scale – NPRS), quality of life (European Quality of Life – 5 Dimensions – 5 Levels – EQ-5D-5L), and Global Perceived Effect (GPE)
Results
The original RCT included a hundred participants and between 91 and 93 of them filled in the outcome measures at 16 weeks. At baseline, the participants had high expectations with 92 out of 100 expecting the treatment effect at 16 weeks to be 5 or 6 on the 7-point Likert scale. They had a mean score of 44.9/60 on the Self-Efficacy Questionnaire, meaning that they had on average higher levels of self-efficacy related to their shoulder symptoms. The Tampa scale revealed, with a mean score of 22.7, that the fear of movement was on the lower end, meaning lower fear of movement. They had shoulder symptoms for 3.3 years on average.

The analyses revealed that:
- Higher self-efficacy at baseline was associated with improved shoulder function, quality of life, and decreased pain at the 16-week follow-up.
- More fear of movement at baseline was associated with increased pain and decreased quality of life at the follow-up of 16 weeks.
- A longer symptom duration was associated with lower levels of quality of life at 16 weeks.
- High expectations of treatment effect at baseline were associated with increased odds of perceiving an important improvement in physical symptoms.
The bold lines were significant after adjustment for all exposure variables.
Questions and thoughts
This analysis found a significant association between several psychological exposure and outcomes in shoulder hypermobility. For good outcomes, your patient with shoulder hypermobility spectrum disorder would ideally have low fear of movement, a shorter symptom duration and higher levels of self-efficacy, and high expectations for physiotherapy treatment.
Fear of movement and self-efficacy are two variables we can try to influence, and this could possibly also influence the expectations for treatment effect. Symptom duration is, of course, not influenceable, however, this sample had a mean symptom duration of 3 years and still managed to improve their perceived shoulder function. Yet, no increased effects on shoulder function were demonstrated. This would mean that these patients, despite having no improvements in the WOSI score, did perceive a positive effect on their physical symptoms. As the longer symptomatology was associated with decreased quality of life, psychological distress should be carefully considered and managed.
When the analysis adjusted for all exposure variables, only the association between symptom duration on quality of life, and high treatment expectations on perceived symptom improvement remained significant.
Talk nerdy to me
As this is a secondary analysis, of course, this study may lack the power to detect the associations with shoulder function. The multiple regression models explained between 30 and 50% of the variance in the outcome variables, meaning that a lot more than just these psychological factors are determining the outcomes. The generalizability of these outcomes is more applicable to women as almost 80% of the included participants were female. But importantly, when a patient comes in who already had received previous treatment and has a long duration of shoulder complaints, they can still achieve good outcomes! Important to note, an association between two variables doesn’t imply causation.
Take home messages
There was a significant association between expectations of recovery, self-efficacy, fear of movement and symptom duration, and better treatment outcomes. Yet, this was a secondary analysis of an RCT, so the results should be cautiously interpreted as no power was calculated for examining these associations.
Reference
LEARN TO DISTINGUISH SHOULDER FACTS FROM FICTION
Awarded World Leading Shoulder Expert Filip Struyf takes you on a 5-Day Video Course to Bust Lots of Shoulder Myths that Prevent you From Delivering the Best Care for your patients with Shoulder Pain

