What is the importance of being able to stand on one foot for 10 seconds?

Introduction
Falling is related to adverse outcomes, especially in older populations. In that way, balance is sometimes viewed as a parameter of health. However, this is not often assessed and as such, it is often not discovered until the balance deteriorates. In this light, the current study examined a simple balance test and wanted to know whether it was associated with all-cause mortality and whether it could give relevant prognostic information beyond demographic, anthropometric, and clinical data. So is there a relation between the 10-second one-leg balance and survival?
Methods
To examine the research question, the study used data from the CLINIMEX Exercise cohort. This cohort was set up in 1994 to examine possible relationships between physical fitness, cardiovascular risk factors, and mortality outcomes. The current study was a prospective cohort using data from 1702 patients of the CLINIMEX cohort. They were aged 51-75 years when they were evaluated first. Anthropometric measurements were obtained and included the measurement of height, weight, and skinfolds. Subsequently, BMI and the weight-height ratio were calculated. Obesity was defined as a BMI of 30 kg/m2 or more. The medical history was obtained by recording the presence or absence of known relevant diseases and the use of medications on a regular basis.
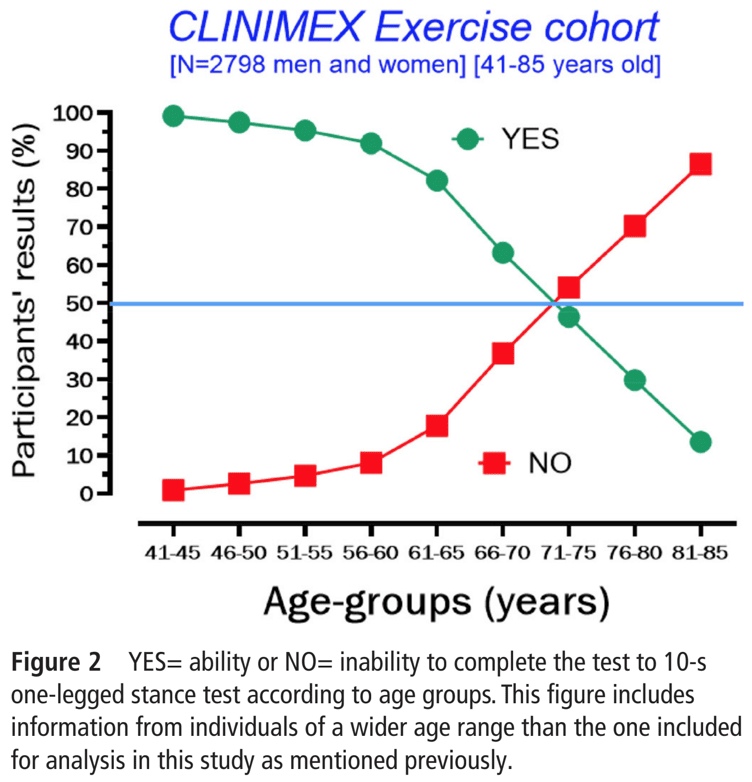
The assessment was continued by having the participant stand on one leg (either left or right, of their choice). Static balance was assessed as the ability to complete 10 seconds in this position. The foot of the other leg was placed behind the standing leg and participants were asked to keep their arms relaxed next to their bodies and to fix their gaze at a specific point on eye level at a 2-meter distance. A maximum number of three attempts was allowed. When participants were unable to hold this position for 10 seconds, they were classified as NO. When participants successfully completed a 10-second stance, they were classified as YES.

Results
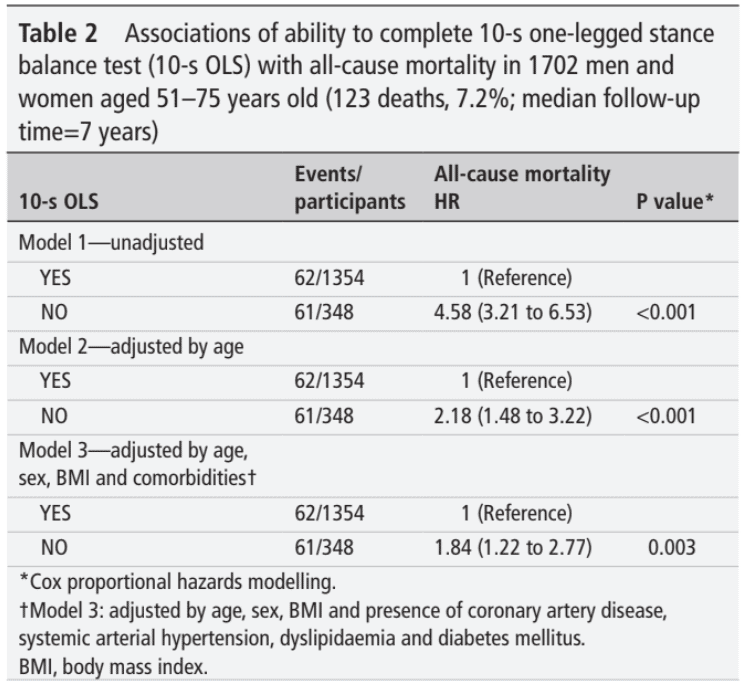
The sample studied was 61.7 (+/-6.8) years old. Most of the participants were male (68%). In total, 348 participants (20.4%) failed to pass the test and were classified as NO. The study showed that the higher the age, the higher the proportion of people failing the test. Over a median follow-up time of 7 years, 123 participants died (7.2%). The results showed that the proportion of deaths was significantly higher in the NO group compared to the YES group. In total, 4.6% and 17.5% of the YES and NO groups died, respectively. Each group had thus approximately 60 people who died, but the NO group was comprised of 348 people, whereas the YES group consisted of 1354 participants. This means that the absolute difference was 12.9% and importantly, there was no difference considering the major underlying causes of death.
Participants who were unable to perform the 10-second leg stand had an unhealthier profile. They had more coronary artery disease, hypertension, dyslipidemia, and obesity. The presence of diabetes mellitus was 3 times more common in the NO group (37.9%) compared to the YES group (12.6%). This difference was statistically significant.
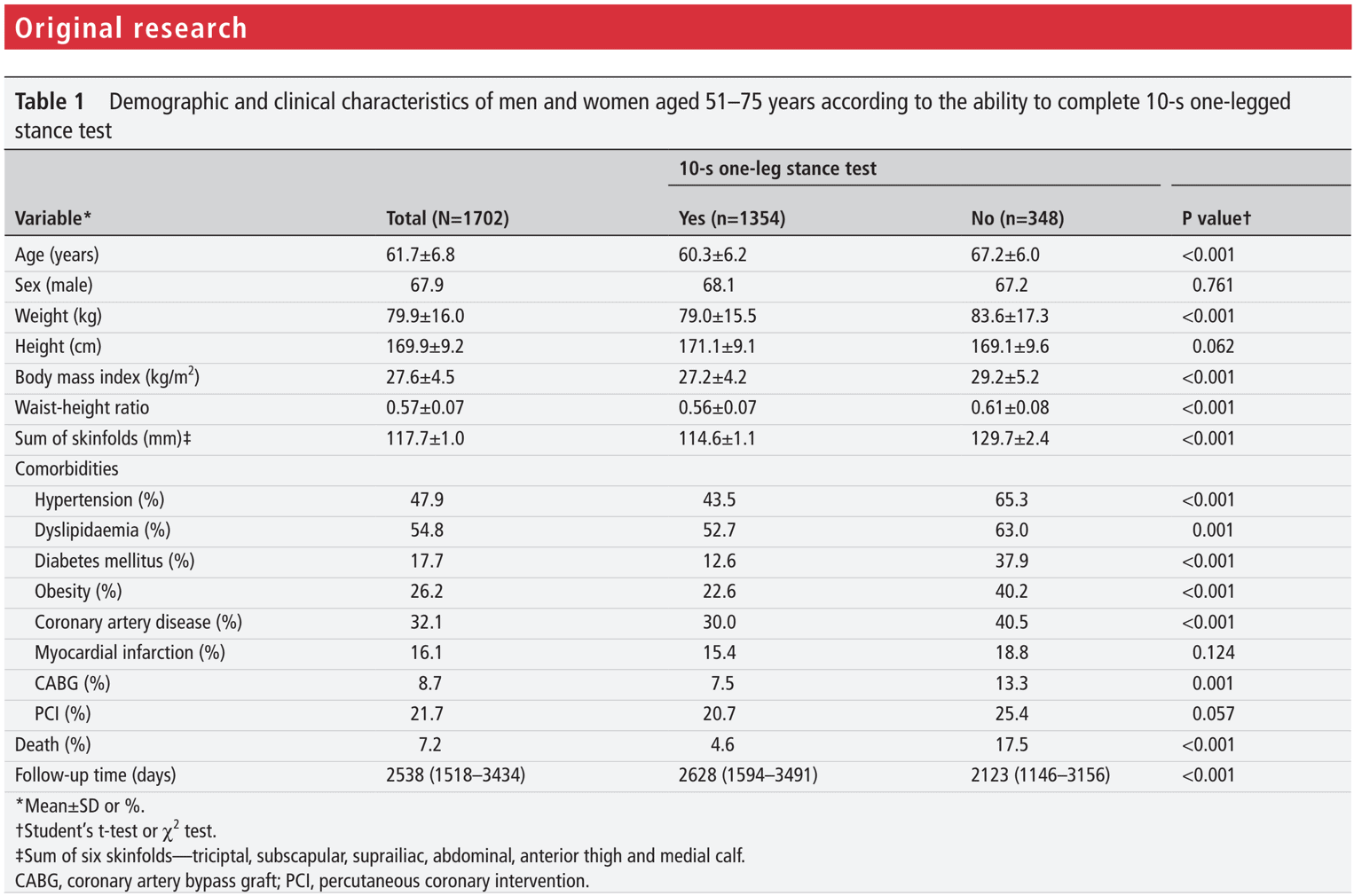
The study also constructed Kaplan-Meier curves to analyze the survival rates in both groups. Striking to see is that the probability of survival decreases quickly in the NO group. The relation between the 10-second one-leg balance and survival prediction is thus existing.
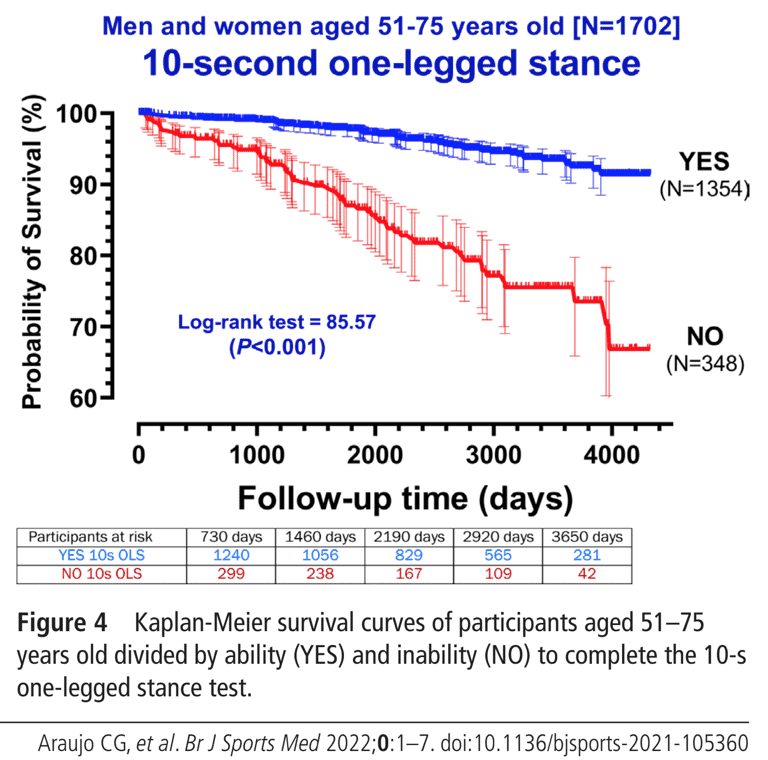
After adjustments were made, the hazard ratios were 2.18 and 1.84 for the age-adjusted and for the age, sex, BMI, and clinical comorbidities-adjusted, respectively.
Questions and thoughts
In this study, results showed that balance is a factor in determining the risk of early death. The ability to complete a 10-second one-leg balance test decreases with aging. However, when adjusted for age and even for other relevant parameters, the risk of dying early was higher among those unable to stand on one foot for 10 seconds. Importantly, this study had high data availability, with less than 1% missing data.
Individuals with unstable gait and/or signs of vestibular or otoneurological dysfunction were excluded. This way, they tried to minimize the influence of balance disorders. Only individuals from the age of 51 to 75 were included in the study as survival curves calculated before data analysis indicated this age range was found to be relevant. The reliability of this test is moderate to good, based on the evidence for one-leg stance tests. A strength of this study was that the median follow-up and the percentage of deaths occurring provided a 92% power to examine the research question. One limitation was that information on a history of falls was missing. Data on activity and exercise patterns, dietary habits, smoking, and medication use were also not available.
Talk nerdy to me
The study showed significant associations between the inability to complete the test and the recorded demographic and anthropometric variables. The highest correlation was found for age. This seems quite logical that age influences balance in the majority of people. However, just above, the age-adjusted HR was still pointing to an increased risk for all-cause mortality in those unable to stand for 10 seconds on one foot. So it is not just about age.
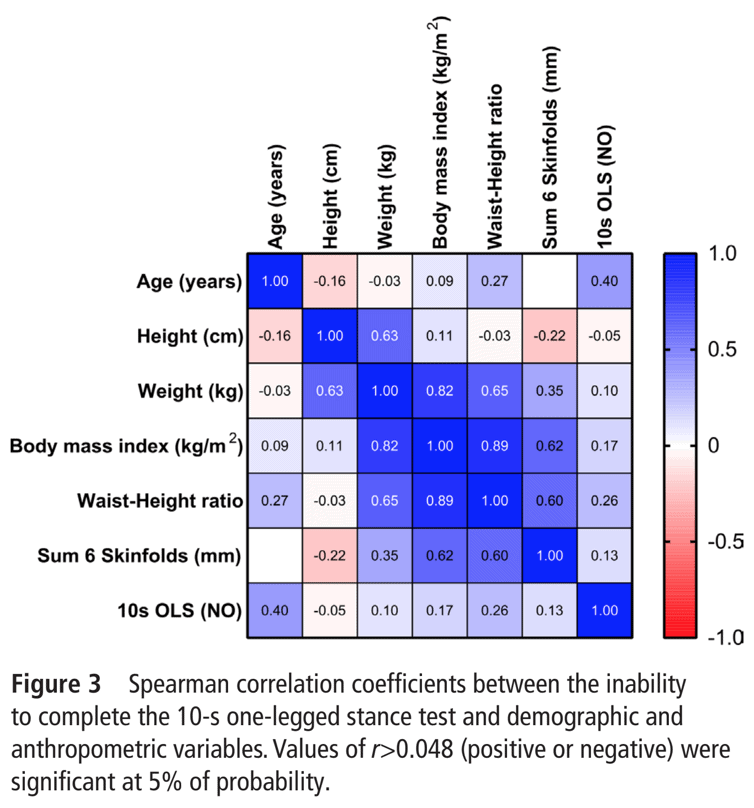
The 10-second one-leg balance and survival test revealed there was a higher percentage of participants with diabetes mellitus in the NO group. This may suggest that these participants had subclinical signs of central nervous system disturbances, highlighting the potential need for balance training interventions in this subgroup of people. Further, in the NO group, there was an association with a high waist-height ratio. This means that a higher waist circumference may be more associated with postural instability and may increase the risk of falls. Furthermore, loss of balance and flexibility together with sarcopenic obesity, which is the presence of obesity characterized by low levels of skeletal muscle mass and high levels of adipose tissue, is detrimental to overall health. The study examined the C-index to know whether the information obtained from the 10-second one-leg stand test could improve the prediction of all-cause mortality. A C-index of 1.0 indicates a perfect prediction of all-cause mortality. With the addition of the results of this test, the model’s prediction increased by 0.01. The net reclassification improvement (NRI) was calculated to examine whether the risk for early death increases when the information of the 10-second one-leg stand test was added to the prediction model. The integrated discrimination improvement (IDI) was calculated to evaluate the capacity to predict early death. Both suggested that the 10-second one-leg test was adding value to the prediction of mortality.
Take home messages
It is normal that balance declines with age. Yet, a better ability to balance on 1 foot for 10 seconds was associated with a lower risk for early death. As such, there is a relation between 10-second one-leg balance and survival. This association was preserved when adjustments for age, sex, BMI, and clinical comorbidities (including a history of coronary artery disease, hypertension, diabetes, obesity, and dyslipidemia) were made. This particularly easy and quick test may be an interesting tool to use for balance evaluation in middle-aged and older adults in practice. The current study did not evaluate the influence of a certain treatment on balance outcomes.
Learn more
Read: The Association of Ankle Plantar Flexor Strength with Balance and Walking Speed
Reference
21 OF THE MOST USEFUL ORTHOPAEDIC TESTS IN CLINICAL PRACTICE
We have comprised a 100% Free E-Book containing 21 of the hands-down most useful orthopedic tests per body region guaranteed to help you reach a proper diagnosis today!

