Cluster Headache | Diagnosis & Treatment All you need to know

Cluster Headache | Diagnosis & Treatment All you need to know
Introduction & Epidemiology
Headaches can manifest on their own but are also a very common symptom in neck pain patients as more than 60% of patients with a primary neck pain complaint report having concordant episodes of neck pain. Therefore it’s essential to find out what kind of headache the patient is suffering from.
To start off let’s differentiate between primary and secondary types of headaches. But what does this mean? Simply put, primary headaches are a “disease themselves” whereas, in secondary headaches, the headache is a symptom of another condition. So primary headaches would be migraines, tension-type headaches & cluster headaches. Secondary type headaches are headaches caused by tumors, hemorrhage, other trauma, TMJ dysfunction, substance overdose, or neck pain aka. The cervicogenic headache.
Now let’s take a closer look at cluster headaches, which are primary types of headaches.
Fischera et al. (2008) conducted a meta-analysis to assess the lifetime prevalence of cluster headache and found low numbers of 0,12% with a 1-year prevalence of 53 per 100,000 persons and the overall sex ratio was 4.3 (male to female). Cluster headache had a 1-year prevalence of 0,054% among the working-aged population in a Swedish cohort (Manzoni et al. 2019)
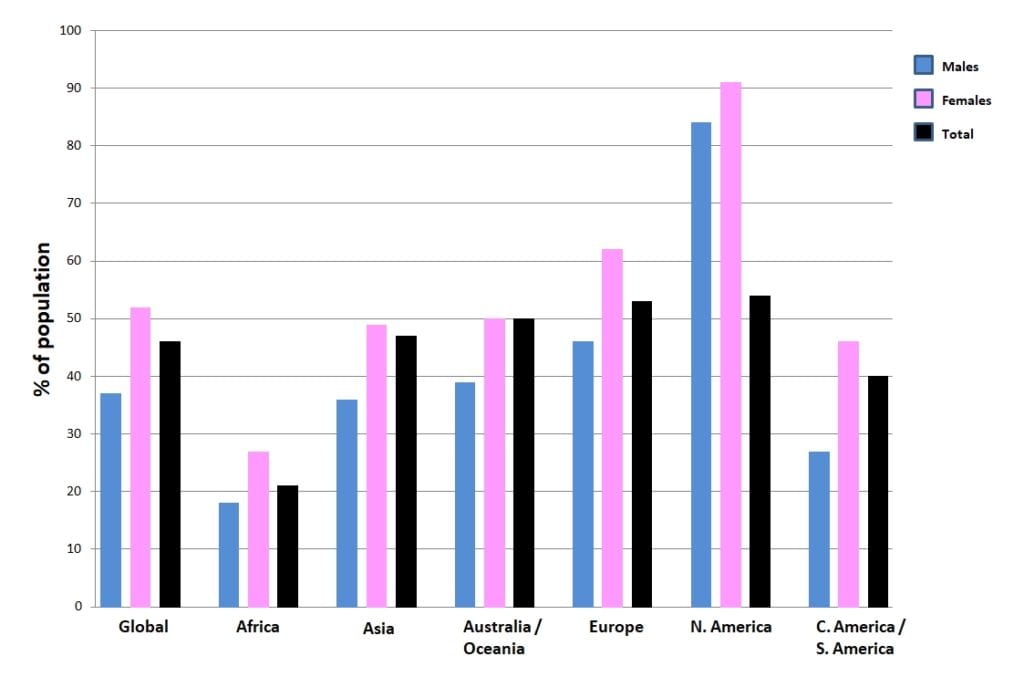
Epidemiology
The following figure shows the prevalence of headaches on different continents around the world:
Follow a course
- Learn from wherever, whenever, and at your own pace
- Interactive online courses from an award-winning team
- CEU/CPD accreditation in the Netherlands, Belgium, US & UK
Clinical Picture & Examination
In order for a headache to qualify as a cluster headache it has to fulfill certain criteria (ICHD-III):
A. At least five attacks need to fulfill criteria B-D
B. An untreated episode lasts 15-180 minutes and shows severe or very severe unilateral orbital, supraorbital, and/or temporal pain
C. It matches either or both of the following:
- at least one of the following signs and symptoms, ipsilateral to the headache:
– conjunctival injection and/or lacrimation
– nasal congestion and/or rhinorrhoea
– eyelid edema– forehead and facial sweating
– miosis and/or ptosis - a sense of restlessness or agitation. There are reports of patients pacing back and forth through the room, banging their heads due to the severe pain.
D. It occurs with a frequency between one every other day and 8 per day
100% Free Headache Home Exercise Program

Follow a course
- Learn from wherever, whenever, and at your own pace
- Interactive online courses from an award-winning team
- CEU/CPD accreditation in the Netherlands, Belgium, US & UK
Treatment
Treatment for cluster headache consists of medication, injections/suboccipital nerve blocks, or intracranial stimulation. We can distinguish between treatment for acute attack and preventative treatment as two facets of cluster headache management. Unfortunately, there are currently no options for physiotherapists to treat patients with cluster headaches.
Currently, only a case study has been published on the combination of endogenous neurostimulation and physiotherapy (Navarro-Fernández et al. 2019).
Acute
100% oxygen therapy is arguably the most well-known method of treating cluster headaches (Obermann et al. 2015). As compared to other types of headaches, cluster headaches are the only condition for which this strategy is a level A recommendation. A minimum of 66% of patients benefit from oxygen therapy. It takes less than ten minutes to take effect. Using oxygen has no risks or adverse effects, making it a great option for treatment. Sadly, oxygen therapy for those with cluster headaches—which can be challenging to obtain—is frequently not covered by insurance.
The only other level A-indicated therapy is triptans. Subcutaneous sumatriptan or nasal spray zolmitriptan delivery of these medications are both options (May et al. 2006). If subcutaneous injections are not tolerated, intranasal triptans might be given on the side opposite the headache. Intranasal sumatriptan (20 mg) and intranasal zolmitriptan (5 mg) are two options. As the onset period of oral medications, in whatever form, is frequently longer than the headache, they are not advised.
Alternative treatments include octreotide, ergotamine, and intranasal lidocaine (with a reported 33% response) (Matharu et al. 2004). Sadly, medication resistance develops in 10% to 20% of people with severe cluster headaches. Patients should be advised to stay away from triggers, particularly alcohol. Patients should be urged to cease smoking even though there is no evidence to suggest that doing so will reduce their likelihood of getting headaches.
Preventive Medicine
The sole tier A suboccipital blockade is advised as a method of cluster headache avoidance. Negative side effects include temporary injection site soreness and mild headaches, both of which are not significant.
The most frequently prescribed prophylactic medication is verapamil (May 2003).
For patients with persistent cluster headaches and those who have episodic cluster headaches for at least two months, it is advised as the first line of preventive treatment (Obermann et al. 2015).
For episodic and persistent cluster headaches, verapamil, which is useful as a preventive medication, is started at 240 mg once daily (Leone et al. 2000). It is advised to perform routine ECGs to check on a patient’s heart health while they are taking this medication. Verapamil has a level C recommendation, despite being widely used by healthcare professionals.
Lithium, valproic acid, melatonin, and intranasal capsaicin are some more pharmaceutical choices (Ekbom et al. 2002).
The effects of electrical stimulation have been extensively studied. The sphenopalatine ganglion, occipital, and vagus nerve are among the areas that are stimulated. The hypothalamus has benefited greatly from deep brain stimulation, which has been particularly effective in treating patients who are drug-resistant (Fontaine et al. 2010). A non-implanted device may offer the option of vagus nerve stimulation (Goadsby et al. 2018).
Want to learn more about headaches? Then check out our following blogs & research reviews:
- Physical Tests for Headaches: Useful?
- The Efficacy of Aerobic Exercise vs. Strength Training in the Treatment of Migraine
- Podcast Episode 031: Headaches with René Castien
References
Follow a course
- Learn from wherever, whenever, and at your own pace
- Interactive online courses from an award-winning team
- CEU/CPD accreditation in the Netherlands, Belgium, US & UK
Finally Learn how to Diagnose & Treat Patients with Headaches


What customers have to say about this online course
- Ryanne Groenewegen - van GulikIdeale online cursus Voor online begrippen en hele sterke cursus. Wordt duidelijk vermeld wat “verplichte” stof is en verdiepende stof. De presentaties van René zijn een beetje statisch gepresenteerd maar benutten de meest essentiële informatie. De toetsen/quiz waren soms vrij moeilijk. Ga daar goed voor zitten.
Toevoeging voor mij zou nog zijn meer casus /case report voorbeelden in de toetsen verwerken en net zoals uitleg bij hcwk palpatie in elk filmpje toelichting en uitleg van handvattingen en richtingen. Al met al echt ideaal het in je eigen tijd te kunnen doen en er bovendien ook veel van te leren!Simon FayersThe confusion of headache diagnose lifted Ive been working many years but always felt that my tool box was a little empty when dealing with headache patients. This course has given me both a theoretical and practical base to build upon in clinical practise. The course is quite heavy on research papers as they are looking to evidence everything that is taught and also perhaps as Rene is primarily a researcher and this is an important area of interest for him. There are plenty of practical videos on testing and treatment.
Really happy i took this course. - Raphael AcohenInteressant, pittig en droog Als algemeen fysiotherapeut vond ik deze cursus inhoudelijk sterk en wetenschappelijk goed onderbouwd. De vele papers en analytische benadering gaven veel diepgang, maar maakten het ook best pittig. Daarnaast kwamen de filmpjes vrij droog over, wat het soms lastig maakte om de aandacht erbij te houden. Visuele praktijkvoorbeelden hadden de leerervaring nog levendiger gemaakt. Toch een waardevolle cursus voor wie echt de diepte in wilMenno SormaniHeadache treatment in clinical practice Wat fijn dat physiotutors de samenwerking is aangegaan met Rene Castien. Heel erg duidelijke cursus met zowel diagnostiek als behandeling bij hoofdpijn.
- Martijn LiebregtsPrima cursus Beste Physiotutors,
De online cursus "Behandeling van hoofdpijn in de klinische praktijk" is mijn eerste cursus welke ik bij jullie afgerond heb. Mijn verwachtingen waren niet al te hoog aangezien deze manier van scholing niet mijn voorkeur heeft. Maar ik moet zeggen dat ik positief verrast was. De cursus is prima te doorlopen, alles zit erg goed, duidelijk in elkaar en je kunt op een prettige manier studeren. Voor mij persoonlijk was het wel erg veel leesmateriaal. Dit is een goede en interessante manier van studeren als je je studietijd zelf wilt invullen.Hayko OosterveldHeadache Treatment in Clinical Practice Weer een goede cursus van Physiotutors: Headache Treatment in Clinical Practice
Goede cursus, met veel (wetenschappelijke) achtergrond informatie en heel bruikbaar voor de praktijk. - Rob van DamHoofdpijnbehandeling in de klinische praktijk Goede cursus, veel geleerd, wel even zoeken voor mij, aangezien dit de eerste x is dat ik een online cursus doe.
Fijn is dat je zelf kunt bepalen wanneer je de lessen volgt.
De opgegeven tijd die voor de cursus staat heb ik wel heel ruim overschreden.
De vertaling naar Nederlands viel me wel tegen, ik heb de cursus toch maar in het Engels gevolgd.
Ik ga in de toekomst zeker nog eens een cursus via physiotutors volgen.RutgerHeadache Treatment in Clinical Practice geweldige course. Veel informatie maar ook super goede behandeltechnieken. Echt een aanrader - Jelle VisserHeadache Treatment in Clinical Practice geweldig. heel veel informatieTodd A.Thorough course with the necessary depth of material Appreciated the level of RCT evidence presented in the lectures.
- Ilse Lammers-VredenbergVeel geleerd maar ook geïrriteerd Mijn ervaring met deze cursus is wisselend. Laat ik voorop stellen dat ik enorm veel geleerd heb en nu helemaal up to date ben met de huidige standaard qua onderzoek en behandeling van hoofdpijn.
Wel kost de cursus heel veel meer tijd dan de 14 uur die er volgens Physiotutors voor staat. Ook zijn de artikelen niet beschikbaar in de cursus; dan moet je eerst een mailtje sturen en dan krijg je een link waar grotendeels de artikelen in staan. Voordat ik dus hier achter was had ik veel tijd aan het zoeken van de artikelen besteed.
Het is goed dat er getest wordt d.m.v. vragen maar deze zijn soms onduidelijk gesteld en hebben niet altijd betrekking op de stof. Ook was er een vraag over een artikel wat niet gelezen hoefde te worden. Kleine dingen die toch irriteren; want je moet uiteindelijk toch je toetsvragen goed hebben.
Het is dat ik een master MT gedaan heb want als algemeen FT was ik vastgelopen op alle wetenschap en bijbehorende onderzoeksmethodieken.maria Kramergoede cursus voor hoofdpijn klachten Een iets wat te wetenschappelijke cursus over hoofdpijnklachten. Maar goed om je te verdiepen in de anatomie en mechanismes rond hoofdpijnklachten te leren. Tweede deel een aantal goede handvaten voor behandeling van deze klachten. - MartyGoed overzicht van hoofdpijn Ik vond het een mooi overzicht van de verschillende soorten hoofdpijn met zeer uitgebreid
Aandacht voor de symptomen, verschillen en diagnostiek.
De filmpjes zijn heel duidelijk. Het gesproken Engels is goed te verstaan of anders is de ondertiteling voldoende.
Wat mij betreft moet je de Engelse taal wel voldoende begrijpen om de gehele cursus inclusief artikelen
Te voltooien. De toetsen zijn niet al tè moeilijk…😉
Een groot minpunt vind ik wel de gebrekkige werking van de website in z’n algemeen. Onoverzichtelijk en in begin lastig te doorgronden..
Groot voordeel is de gunstige prijs gemiddeld per accreditatie punt. 👍Wouter LinschotenInteressant, overzichtelijk en fijne leerstof! De manier waarop deze cursus in elkaar is gezet is fantastisch. Het is ontzettend overzichtelijk en geeft een goed beeld van de structuur en vooruitgang in je cursus. Bovendien Zijn de video-lectures en vooral de uitleg oefeningen zoals we gewend zijn van Physiotutors: Ontzettend goed gemaakt en duidelijk. Alles is bovendien zeer uitgebreid en goed onderbouwd met uitgebreide literatuur. Ik ga zeker weer een cursus van ze doen. Keep up the good work! - EricOnmisbaar als behandelaar van hoofdpijn Wanneer je meer inzicht in de achtergrond van hoofdpijn wilt krijgen, behandelmethodens en technieken dan is deze cursus onmisbaarRichard PamboerLeerzame cursus Fijn om zelf te kunnen bepalen wanneer je wil studeren. Goede opzet van de cursus.
Grootste minpunt was de slechte vertaling in de ondertitels, verder prima! - Christine Petrides, PhysiotherapistClear, structured teaching that improved my reasoning. I loved learning about different headache types and how to organize my clinical reasoning. The lecturer explained everything in a clear, structured way, and the downloadable resources will be useful for a long time. Highly recommended.Julie VermeerenInteressante en uitgebreide cursus Duidelijke cursus waarmee je direct aan de slag kunt in de praktijk. Veel wetenschappelijke onderbouwing.
Je hebt onbeperkt de tijd om de cursus te volgen, ideaal omdat je daarmee zelf kunt bepalen wanneer je de cursus wil volgen.
Daarnaast kun je dus ook altijd terug de cursus in om wat terug te lezen. Aanrader! - Lech KowalskiInformatieve cursus met zeer veel wetenschappelijke onderbouwing Voor manueeltherapeuten is de cursus goed te doen en te begrijpen. Voor fysiotherapeuten komt er wel wat kennis voorbij die als complex/ingewikkeld kan worden ervaren. De presentaties zijn duidelijk, hoewel er soms misschien een overzichtje ontbreekt. Wat fijn is dat je de presentatie kan versnellen tot 2x zo snel, zodat je zelf het tempo waarmee je de informatie tot je krijgt kan bepalen. Daarnaast is het mogelijk om de tekst van de presentatie ernaast te houden, zodat je mee kan lezen met wat er gezegd wordt. Ondertiteling is in veel talen beschikbaar, al lijkt er soms een foutje in de vertaling te sluipen (cervical wordt bijvoorbeeld vertaald als baarmoeder). Desondanks is het vanwege de context wel duidelijk te volgen.
De cursus heeft een goede opbouw, stukje tekst/leren/presentatie en daar dan een quiz over. De Quizjes zijn best pittig, gemiddeld 1 minuut per vraag, dus je moet echt wel de presentaties en artikelen gelezen/gevolgd hebben, omdat sommige vragen anders niet te beantwoorden zijn. Daarbij zijn deze in het Engels, dus je bent soms al zeker 30sec verder als je de vraag en antwoorden gelezen hebt en begrijpt.
Wat deze cursus heel fijn maakt:
- Eigen (onbeperkte) tijd dat je deze kan volgen
- De hoeveelheid KRF-punten t.o.v. de prijs van de cursus is écht goed
- Je krijgt weer meer inzicht in de laatste stand van zaken m.b.t. het behandelen van hoofdpijn
- Je krijgt een aantal casuïstieken waar je mee aan de slag gaat
Wat beter zou kunnen:
- De presentaties iets geanimeerder/interactiever proberen te geven, soms is het een beetje droge ingewikkelde materie
- Iets meer duiding geven aan sommige onderwerpen die voor de (master) manueeltherapeut bekend zijn, maar waarschijnlijk wat minder voor de fysiotherapeut
Aanrader?
Zoals veel in dit vakgebied is de voertaal Engels, zo zijn artikelen, de presentaties (wel met ondertiteling in taal naar keuze) en de quizjes in het Engels. Wanneer je daar niet comfortabel mee bent, zou ik deze cursus niet aanraden. Collega-manueeltherapeuten zal ik deze cursus zeker wel aanraden!Larsinformatieve cursus met mix van wetenschappelijke artikelen en presentatie De cursus is duidelijk en logisch gestructureerd. De inhoud wordt middels een mix van wetenschappelijke artikelen, presentatie en praktijk skills uitgelegd, hierdoor wordt het makkelijker om de inhoud te begrijpen en onthouden. De lengte van de presentaties is prima, zodat je niet de aandacht/focus verliest.