Different Trajectories of Low Back Pain and Degenerative Imaging Findings in Young Adults

Introduction
This study examined the association between low back pain trajectories and MRI findings. To do so, it used data from the RAINE study, an intergenerational public health study in Australia. Previous data from this study have identified different trajectories of low back pain in young adults. The purpose of the current study was to examine the association between these trajectories and the presence or absence of lumbar spine MRI findings. By collecting data from young adults, the study aimed to limit the finding of coincident positive MRI findings, as a young population typically shows fewer abnormalities on imaging compared to older populations.
Methods
A cross-sectional analysis of data gathered from the RAINE study for individuals between the ages of 17-22 years was conducted. A previous study identified 4 low back pain trajectories in these participants over the course of 5-years. At the ages of 17, 20, and 22 years, these people were asked about the presence of low back pain over the last month using the Nordic musculoskeletal questionnaire. The impact of low back pain was assessed using data on seeking care, the use of medication, time off school/work, modifying physical activities, and or activities. The 4 trajectories found were:
- Consistently low prevalence of low back pain and impact
- Decreasing prevalence and impact
- Increasing prevalence and impact
- Consistently high prevalence and impact
In total, 78 participants from the group with consistently high prevalence and impact of low back pain were included. These were the “cases”. For every low back pain case, a matched control was sought.
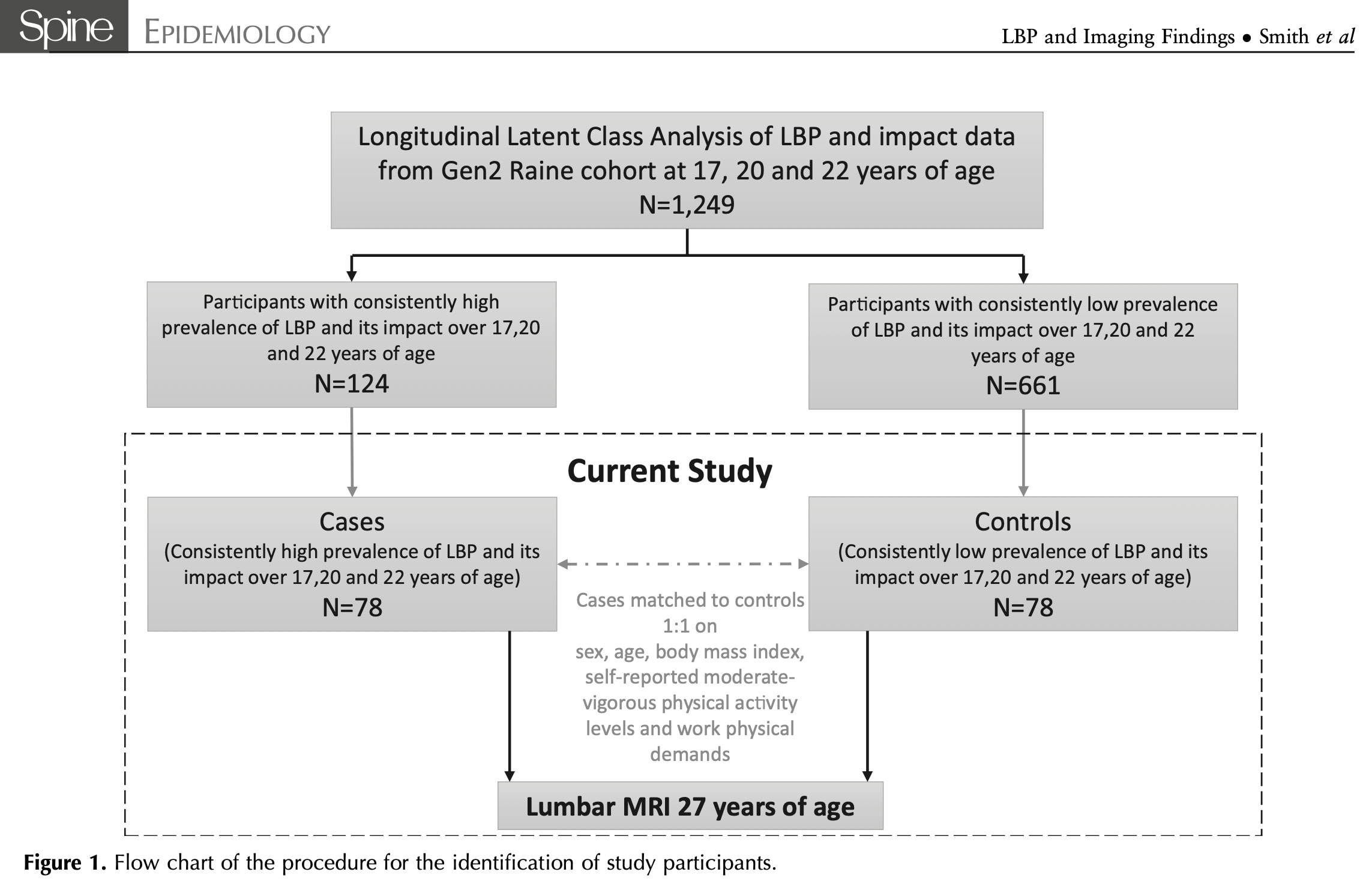
These participants all underwent a lumbar MRI scan and completed the Roland Morris Disability Index, personal impact of low back pain, and a 0-10 Numeric Pain Rating Scale. The Roland Morris index ranges from 0-24 with 24 representing high disability. The personal impact of low back pain ranges from 8-50 with higher scores representing higher impact.
Results
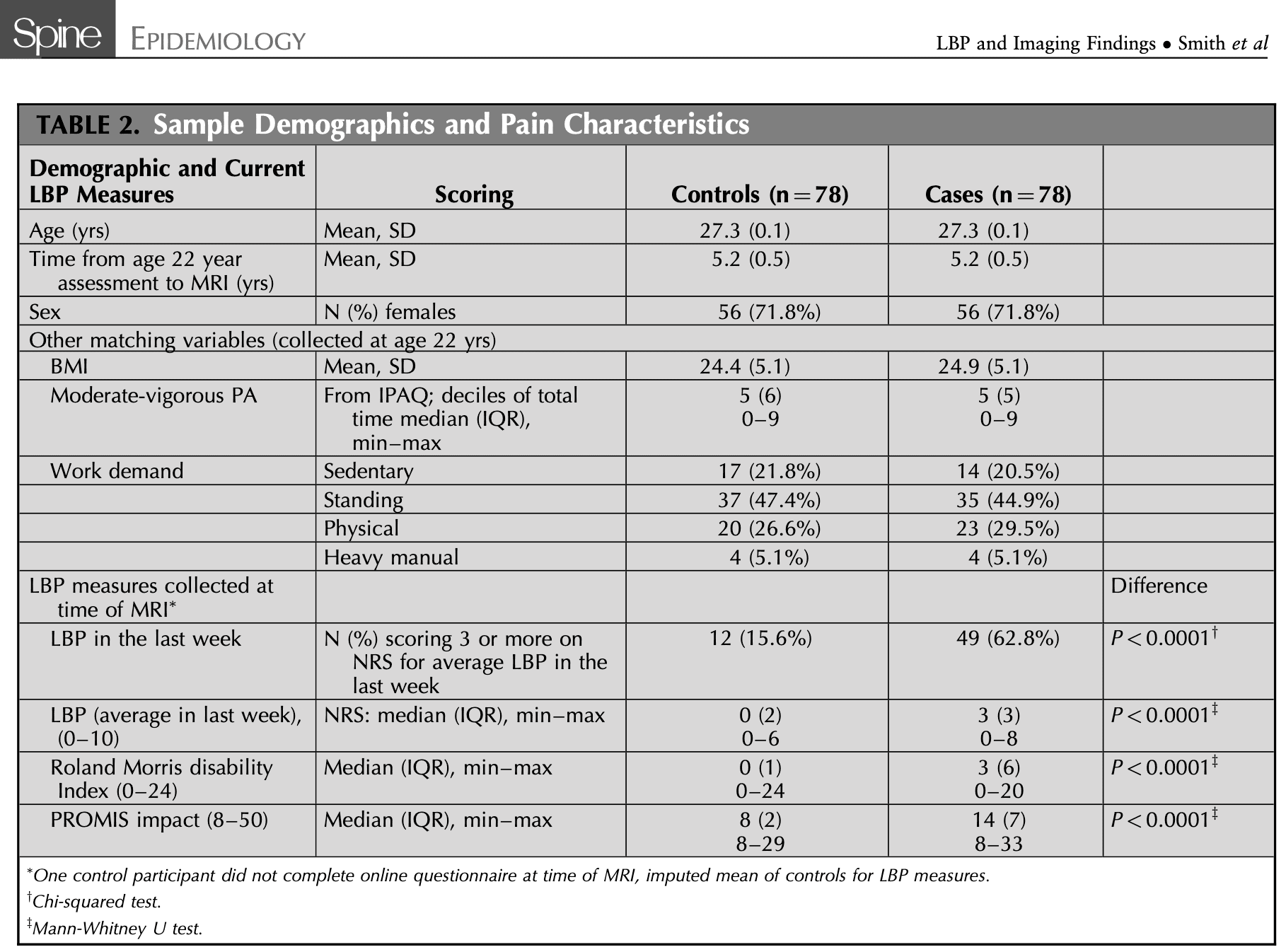
Seventy-eight cases and 78 matched controls were included. The participants were comparable at baseline but logically differed significantly in the presence of low back pain in the last week, the Roland Morris Disability Index, and personal impact of low back pain.
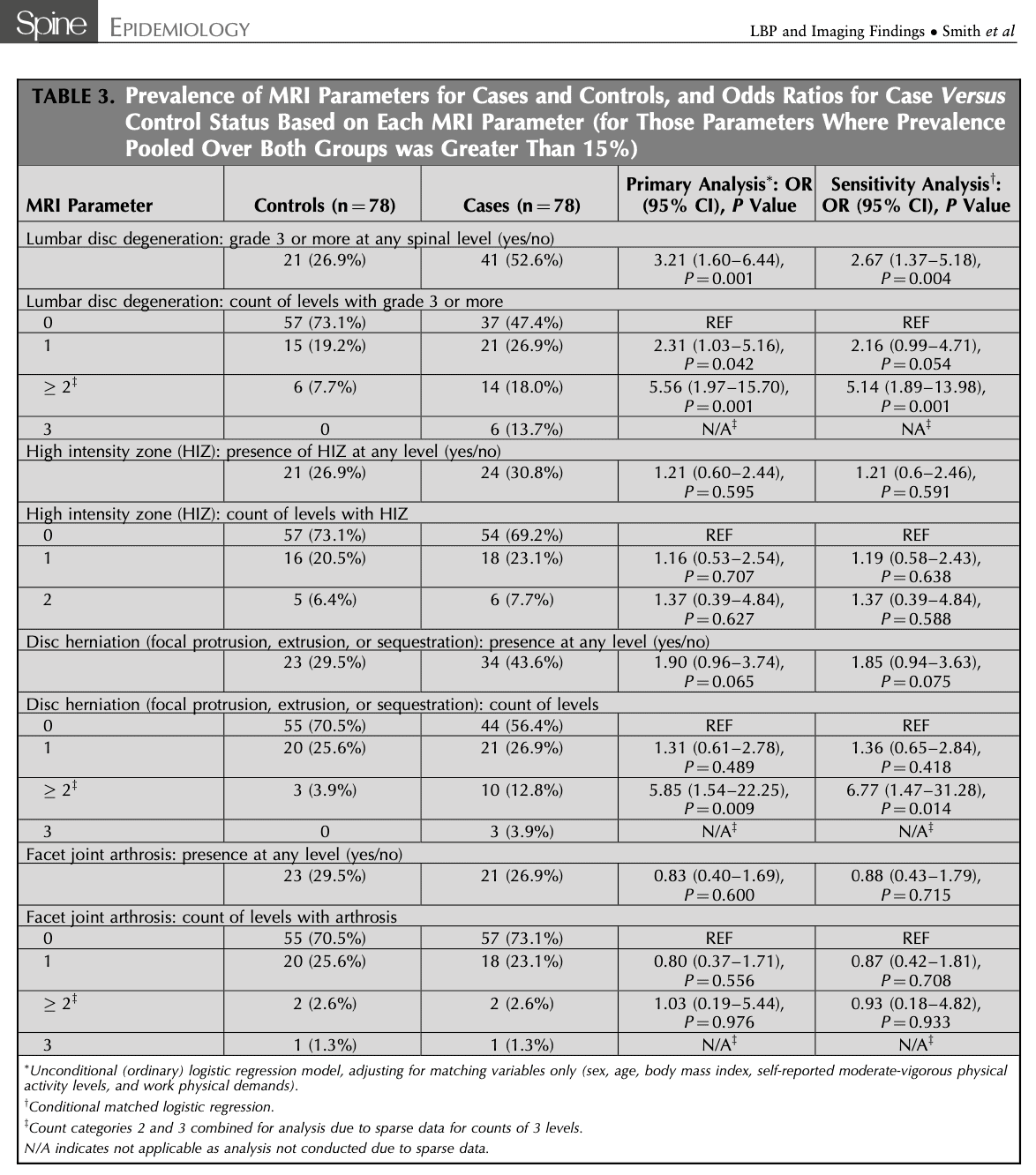
The results revealed that the odds of being a case were significantly higher in the presence of lumbar disc degeneration of grade 3 or higher at any spinal level. The odds were even higher in case two or more spinal levels were affected.
The odds for being a case were higher in case a lumbar disc herniation was present at any level and even more when the herniation was present in 2 or more levels. Such a difference was not found for the presence of facet joint arthrosis, nor when the number of levels with facet joint arthrosis was considered.
Questions and thoughts
This review identified differences in the likelihood of MRI findings between cases with consistently low and high prevalences of low back pain and impact. However, the cross-sectional design of the study does not allow to infer causation, those with high prevalence and impact over a 5-year course had higher chances of abnormal MRI findings. However, table 3 reveals that those with consistently low prevalence and impact of low back pain also could have abnormal MRI findings, albeit sometimes to a lesser extent. The presence of an abnormal finding can therefore not be considered to diagnose someone with low back pain. So remember to always treat the person, and not their MRI!
What was interesting about this study was the inclusion of young people. Generally, compared to an older sample, they are less likely to demonstrate abnormal MRI findings. Another interesting thing about this study is the inclusion of participants with low back pain over a sustained period in their lives, and not at a single point in time.
The definition of the abnormal findings can be seen in the table below. Note that this study defined a disc herniation as the presence of a protrusion, extrusion, or sequestration of a lumbar intervertebral disc. Yet, a protrusion cannot be defined as a real herniation as the nucleus pulposus does not break through the annular ring of the intervertebral disc.
Talk nerdy to me
A very important conclusion is that due to the nature of this study, it is not possible to draw conclusions about causal relationships. There is an association between those with consistently low prevalence and impact of low back pain and the higher likelihood of abnormal MRI findings. But the association says nothing about causation. This needs to be investigated in other research designs. The cross-sectional study also gives us information about this association at one specific time point. Although the prevalence and impact of low back pain in the different trajectories were recorded over a 5-year period, the association with imaging findings was recorded only at the time of the MRI. We cannot say anything about an evolutionary link because we do not know whether the abnormal findings on MRI were already present at the beginning of the 5-year period. Likewise, the results don’t give us information about possible treatments, or environmental and lifestyle factors that may have had a spell on the association found here.
Fortunately, the RAINE study found that most people (53%) were in the 5-year trajectory of low prevalence and impact of low back pain. Only 10% were in the 5-year trajectory of high prevalence and impact of low back pain. Fifteen and 22% of people had decreasing and increasing prevalence and impact of low back pain over these 5 years, respectively. This information shows that fortunately, few young people experience a significant burden of low back pain over a 5-year period. However, although there was a large difference between the prevalences in both groups studied (low versus high prevalence and impact of low back pain), the fact that each “case” with a high 5-year impact of low back pain was paired with a “control” with a low 5-year impact makes it possible to compare people with different trajectories despite the fact that the prevalence rates of low back pain and their course in these trajectories were very different.
Each sample included 78 participants, and although this is not a large number, the study was able to show relatively high odds ratios. Inter-rater reliability was good for finding disc degeneration (kappa 0.855), but only moderate for the presence of a disc herniation and low for the presence of facet joint osteoarthritis (kappa values 0.588 and 0.239, respectively). Therefore, I prefer to use only the odds ratios found for disc degeneration because they were established for the MRI findings with more agreement among reviewers. The relationship between MRI parameters and case versus control status was only statistically investigated where the prevalence of the MRI parameter pooled over the case and control groups was >15%. This limits the number of associations studied and thereby limits the possibility of finding false positive associations.
Take home messages
There is an association between those with consistently high prevalence and impact of low back pain and the higher likelihood of abnormal MRI findings. Those with a history of disabling low back pain over a 5-year period had higher odds of finding abnormal findings on MRI. The association was even stronger in case more lumbal levels were affected. The inter-rater reliability was highest for the finding of disc degeneration. The cross-sectional analysis is not able to draw causal conclusions but may suggest that lumbar disc degeneration may be an important contributing factor to low back pain in young people.
Reference
MASSIVELY IMPROVE YOUR KNOWLEDGE ABOUT LOW BACK PAIN FOR FREE
5 absolutely crucial lessons you won’t learn at university that will improve your care for patients with low back pain immediately without paying a single cent

